

Treatment Adherence in People Living with hiv: Relationship between an Explanatory Model, Motives, and Practices
Adherencia al tratamiento en personas que viven con ViH: vínculos entre el modelo explicativo, los motivos y las prácticas
Adesão ao tratamento em pessoas vivendo com HiV: relações entre um modelo explicativo, motivos e práticas
 Contribution: conceptualization; methodology; investigation; formal analysis; writing the original draft; reviewing and editing
Contribution: conceptualization; methodology; investigation; formal analysis; writing the original draft; reviewing and editing
 Contribution: conceptualization; methodology; investigation; formal analysis; writing the original draft; reviewing and editing
Contribution: conceptualization; methodology; investigation; formal analysis; writing the original draft; reviewing and editing
Treatment Adherence in People Living with hiv: Relationship between an Explanatory Model, Motives, and Practices
Revista Ciencias de la Salud, vol. 19, no. 3, 2021
Universidad del Rosario
Received: 19 november 2019
Accepted: 25 may 2021
Additional information
To cite this article: Almanza-Avendaño AM. Gómez_San Luis AH. Treatment Adheence in People Living with HIV: Relationship between an Explanatory Model, Motives, and Practices. Rev Cienc Salud. 2021;19(3):1-21. https://doi.org/10.12804/revistas.urosario.edu.co/revsalud/a.10721
Abstract: Introduction: The concept of adherence recognizes that not all patients passively accept treatment and suggests a more horizontal relationship between patients and healthcare personnel. The objective of this study was to identify an explanatory model, motives, and practices to ensure treatment adherence in people living with human immunodeficiency virus (HIV) in the state of Tamaulipas, Mexico. Materials and methods: The study was conducted in accordance to the Grounded Theory. Semi-structured interviews were conducted with patients who attend specialized public services for HIV. Results: The patients construct an explanatory model that parsimoniously integrates knowledge regarding HIV infection, antiretroviral therapy, and adherence; it is based on both the information received by patients from healthcare services and their experience with the condition. The model is also linked to motives, such as maintaining health, staying alive, and taking care of oneself for others, that promote adherence. Conclusion: The explanatory model and motives guide the development of pharmacological and nonpharmacological adherence-promoting practices. Healthcare services need to addres these elements for the promotion of adherence over time.
Keywords: Treatment adherence and compliance, self-care, healthy lifestyle, HIV, antiretroviral therapy.
Resumen: Introducción: el concepto de adherencia reconoce que no todos los pacientes aceptan pasivamente el tratamiento y sugiere una relación más horizontal entre el paciente y el personal de salud. El objetivo es identificar el modelo explicativo, los motivos y las prácticas para la adherencia al tratamiento que emplean personas que viven con VIH en el estado de Tamaulipas (México). Materiales y métodos: el estudio se realizó a partir de la teoría fundamentada. Se llevaron a cabo entrevistas semiestructuradas con pacientes que acudían a servicios públicos especializados en VIH. Resultados: los participantes elaboran un modelo explicativo que integra en forma parsimoniosa conocimientos sobre la infección por VIH, el tratamiento antirretroviral y la adherencia, y que se basa tanto en la información que reciben de los servicios de salud como de su experiencia con el padecimiento. El modelo se vincula con motivos para la adherencia, como mantener la salud, seguir viviendo y cuidarse para los demás. Conclusiones: el modelo explicativo y los motivos orientan el desarrollo de prácticas para la adherencia farmacológica y no farmacológica. Los servicios de salud requieren atender estos elementos para la promoción de la adherencia a través del tiempo.
Palabras clave: cumplimiento y adherencia al tratamiento, autocuidado, estilo de vida saludable, VIH.
Resumo: Introdução: o conceito de adesão reconhece que nem todos os pacientes aceitam passivamente o tratamento e sugere uma relação mais horizontal entre o paciente e o pessoal de saúde. Objetivo: identificar o modelo explicativo, motivos e práticas de adesão ao tratamento utilizados por pessoas vivendo com HIV no estado de Tamaulipas, México. Materiais e métodos: o estudo foi realizado com base na Teoria Fundamentada. Foram realizadas entrevistas semiestruturadas com pacientes atendidos em serviços públicos especializados em HIV. Resultados: os participantes elaboraram um modelo explicativo que integra parcimoniosamente conhecimentos sobre infecção pelo HIV, tratamento antirretroviral e adesão; e que se baseia tanto nas informações que recebem dos serviços de saúde quanto na sua própria experiência com a doença. O modelo está atrelado aos motivos de adesão, como manter a saúde, continuar vivendo e cuidar do outro. Conclusões: o modelo explicativo e os motivos norteiam o desenvolvimento de práticas de adesão farmacológica e não farmacológica. Os serviços de saúde precisam abordar esses elementos para promover a adesão ao longo do tempo.
Palavras-chave: cumprimento e adesão ao tratamento, autocuidado, estilo de vida saudável, HIV, tratamento antirretroviral.
Introduction
The precursor of treatment adherence is the concept of compliance, which refers to the degree to which a patient follows the medical recommendations related to medication use and lifestyle changes. However, this concept has been criticized because it establishes a hierarchical relationship between physicians and patients by assuming that medical recommendations are adequate and treatment failures are due to patient noncompliance (1).
Although patients may passively accept drug prescription, they generally assess its costs and benefits based on health expectations, side effects, the psychosocial impact of the treatment, and its complexity and interference with daily life as well as finances. Based on this assessment, patients may accept the treatment, actively modify it after evaluating it, or reject it (2).
The concept of adherence recognizes that not all patients passively accept treatment; therefore, it proposes a more horizontal relationship between patients and physicians (1). Although the concept provides greater patient autonomy, it has been pointed out that it remains prescriptive since it does not necessarily imply collaboration or joint decision making (2). In addition, the proposal of the concept of adherence is limited by the persistence of the hegemonic medical model in the public sphere, which emphasizes individualism, the asymmetrical relationship between physicians and patients that does not enable the establishment of collaborative strategies, and the subordinate and passive participation of the patient in health-related decisions as well as bureaucratism and reduced responsibilities in providing care (3,4).
Despite these criticisms regarding the concept of adherence, it is widely used in the field of care for people living with human immunodeficiency virus (HIV), referred to as patients throughout the text. Because antiretroviral therapy has increased the duration of survival and improved the quality of life of patients, greater interest has been placed on pharmacological adherence, which focuses on the use of medications according to medical prescription. Low adherence to antiretroviral therapy decreases drug concentration in the body; limits its effectiveness; and favors viral replication, resistance to treatment, and viral rebound. In addition, it causes a decrease in CD4+ cells, thereby increasing the risk of morbidity and mortality (5).
Previous studies that focused on the perspective of people living with HIV have identified several facilitators of adherence, such as changes in the health status, beliefs about the condition and treatment, emotional state and the acceptance of HIV, motives such as the desire to live and take care of their health, the use of strategies to remember to take the medications, management of side effects, life style adjustment, having support networks, and maintaining a collaborative relationship with healthcare services (6,7). One criticism of these studies is that they describe a set of facilitators of adherence but do not link them to each other or reveal which are the most relevant ones in order to assist healthcare services in establishing priorities when intervening to promote adherence.
Empirical models of adherence in people living with HIV emphasize different elements that contribute to the process and focus on individual variables that are under their control. One study emphasizes the role of autonomous motivation, which requires patients to not only comply with medical advice but also communicate their beliefs about treatment, actively participate in treatment planning, and be empowered to make decisions regarding care. In addition to having autonomous motivation, the patients are required to perceive themselves as competent to follow the recommendations of medication use (8).
Similarly, it has been found that adherence is favored when the patient possesses the functional skills required for medication use and is motivated and has lower levels of stress when facing events related to the disease or results of the treatment (9). Other studies prioritize the role of self-efficacy, beliefs about treatment efficacy, and the development of a medication-taking habit as well as acceptance of the condition (10,11).
Previous studies highlight the role of motives and behaviors in the adherence process. In this study, it is considered that the understanding of this process can be deepened by incorporating explanatory models. These are constructs about an episode of illness and its treatment, which are employed by those involved in the healthcare system (12). These contain explanations of the biological disease and its treatment, provide guidance to make decisions regarding available treatments, and provide personal and social meanings to the experience of the disease. The explanatory models of the patient and healthcare personnel are continuously interchanged with several possible outcomes—both are maintained by the patient; the healthcare personnel’s model is integrated in a distorted form, while the patient’s model is the one that prevails; only one model is maintained; or a new explanatory model is created (12).
Tamaulipas is located in northeastern Mexico on its border with the United States. By the end of 2018, 3,179 cases of people being registered as HIV-positive had been reported in the state (3.8 % of the national total, ranking ninth); of which, 28.1 % were women (13). A low adherence rate of 52 % was reported in a study in Tamaulipas, whereas another study in Mexico reported a rate of 68.5 % (14,15). Furthermore, it has been stated that the level of pharmacological adherence depends on the indicator used; in a national study, levels of 86.8% werw with a 4-day adherence, which dropped to 55% when the adherence index was used (16).
The purpose of this study is to understand the explanatory model that patients elaborate about their condition and consider it as a framework that guides adherence-promoting practices. We also seek to identify the motives that promote adherence and explore how they are linked to the explanatory model and adherence-promoting practices from an integral perspective. This includes both practices associated with medication use (pharmacological adherence) and those linked to healthcare in different areas (nonpharmacological adherence).
Materials and methods
This study was conducted in HIV specialized healthcare centers in the state of Tamaulipas, Mexico. It was developed in accordance to the Grounded Theory for methodological orientation, assuming that theories are not discovered but constructed through the evaluation of past and present interactions with people, perspectives, and research practices (17). Participants were selected by theoretical sampling in order to contrast the findings by epidemiological group (women, homosexual men, and heterosexual men) and region (north, center, and south of the state). All participants were adults, had been on antiretroviral therapy for at least one year, and attended the Ambulatory Center for the Prevention and Care of AIDS and Sexually Transmitted Infections (CAPASITS). The project was approved by the Ministry of Health of the state of Tamaulipas and by the Research Ethics Committee of the Consolidated Academic Body,“Migration, Development and Human Rights” (UAT-CA-73) of the Autonomous University of Tamaulipas. The study adheres to the Declaration of Helsinki and Resolution 8430 of 1993 of the Colombian Ministry of Health.
The project was first presented to the authorities of the Ministry of Health and then to the directors of the CAPASITS. Patients were contacted by healthcare personnel and personally invited to participate. The purpose of the study was explained to them, and their informed consent was obtained, which guaranteed the confidentiality of information and anonymity of their participation. Twenty-eight patients participated in the study; only three people declined to participate since the length of the interview or the timing of the interview interfered with their daily activities. Data were collected in the CAPASITS clinics or consultation rooms. Only participants and researchers were present during data collection.
The interviews were conducted by both the authors. A semi-structured interview guide was used and tested in a pilot study. A single interview was conducted with each participant. The interviews were audio-recorded and field notes were prepared at the end of the interviews. The duration of the interviews ranged from 40 min to 1 h. The interviews were conducted until theoretical saturation was obtained.
The audio-recorded interviews were used for further transcription and analysis by the researchers. By requesting consent for recording, individuals could decide whether or not to participate in the interviews without affecting their relationship with the healthcare services. The names of participants were not recorded or mentioned during the interviews to ensure anonymity. It was established that the researchers would be the only people with access to the recordings, and they would be deleted after transcription. Any personal information associated with the participants was removed from the transcripts to avoid identification. It was also noted in the consent that in case the material has to be cited, pseudonyms would be used as an additional measure to guarantee anonymity. Another reason why the interviews were recorded is that in a second stage of the study, the voices of patients and practices would be incorporated for designing an intervention for the promotion of treatment adherence; this was also stated in the informed consent.
Coding was carried out by both the authors independently. The categories emerged inductively from the data. Software MAXQDA version 12 was used for the computer-assisted analysis. Through the program, initial notes were expounded, and the processes of open, selective, and axial coding were carried out in order to identify the main categories and subcategories related to the elements that favored the adherence process. Subsequently, the co-occurrence of subcategories across cases was analyzed to identify the degree of association. Finally, theoretical coding was carried out manually to integrate the categories and subcategories in a process that showed the interaction between the explanatory model, motivations, and practices that facilitate adherence.
Results
Ten women and 18men participated in the study—10 were from the northern zone, 10 from the central zone, and 10 from the southern zone of Tamaulipas. Participants had an average age of 42.2 years, ranging from 21 to 61 years. Nineteen participants (including both men and women) identified themselves as heterosexuals, 4 as homosexuals, 4 as gays, and 1 as bisexual. With respect to education, 6 received baccalaureate education, 8 received education up to the university level, 11 up to the high school level, and 3 up to the elementary school level. At the time of the interview, four participants were unemployed, six were employed at home and the rest were in paid employment. Fifteen participants were single, 3 were married, 6 were cohabiting, and 4 were separated or divorced.
Seventeen participants had children (between 1 and 5). On an average they had been living with HIV for 6.32 years (ranging from 1 to 24 years).
Participants had been under treatment for an average of 5.62 years, with a range of 1–24 years. Patients took 2.72 pills per day on an average, with a range of 1–6. Since initiation, 9 patients interrupted antiretroviral therapy (from less than a week to a maximum of 6 months) and 18 experienced changes in their treatment regimen.
The level of pharmacological adherence, i.e., adherence focused on medication use, was measured through two indicators, i.e., 4-day adherence and adherence index (16). Four-day adherence is an indicator based on the ratio between the number of doses prescribed and doses not taken in the previous 4 days. In contrast, the adherence index does not just take into account this ratio but also the adherence to the schedule and the particular instructions of medication use in the last 4days and the time passed since a dose was missed. On measuring 4-day adherence, 5 and 23 participants were found to have an adherence of >95 % and 100 %, respectively. The average adherence rate was 96.51 %, ranging from 75 % to 100 %. However, when adherence index was measured, only 15 were found to have an adherence ≥95%. With this indicator, the average adherence rate decreased to 92.4%, with a range 66.2% to 100% (Figure 1). Based on the last laboratory study performed, 26 participants reported having a viral load at an undetectable level.

The next two sections describe the most relevant categories and subcategories obtained from the qualitative analysis, which represent the elements of the explanatory model, motives that promote treatment adherence, and pharmacological and nonpharmacological adherence-promoting practices. When presenting the findings, the number of cases (n) in which the corresponding subcategories appear is indicated.
Explanatory model of the condition
The main sources from which the participants obtained information regarding HIV infection, treatment, and adherence were healthcare services (n=21), followed by manual search (n=9) either in print or digital media, and to a lesser extent from members of their support network (n=5).
The explanatory model of the condition can be differentiated into several areas. First, patients construct a meaning of HIV infection. There are different conceptions among patients regarding what it does in the body: it affects the immune system (n=15), impairs health (n=9), and can replicate (n=4) or stay dormant (n=2). While the explanatory model is influenced by biomedical discourse, patients also develop a personal or intimate meaning of the condition. HIV infection can symbolize “continuous battle” (n=12), adoption of a healthy lifestyle (n=10), maintenance of a “normal” life (n=9), or “living with stigma” (n=6).
Complementarily, a part of the explanatory model is linked to treatment. Patients consider that antiretroviral therapy primarily controls the virus (n=19) but indirectly strengthens the immune system (n=13). When evaluating the consequences anticipated by patients for not following the treatment, it was found that they most frequently expressed deterioration of health (n=21), in addition to the virus becoming resistant (n=14), or active (n=9) as the consequences. To a lesser extent they mentioned that nothing happens (n=3), or they did not know the consequences (n=3). Regarding side effects, patients mainly identified those that they had experienced, such as gastrointestinal (n=8), mental health (n=7), internal organ-related (n=6), neurological (n=5), or muscular problems (n=4). To a lesser extent they mentioned the presence of problems related to skin (n=3), general health (n=3), fat distribution (n=2), or metabolism (n=2). Some patients mentioned not knowing about the side effects (n=6) or that they only occurred at the beginning of treatment (n=6).
In the explanatory model, patients also develop knowledge about treatment adherence. It mainly involves the practice of medication intake (n=18), indicating the importance of the medication in health care. Another element mentioned was the responsibility of taking care of oneself (n=15). Notably, some mentioned not knowing what adherence was (n=3) or that it represented dependence toward treatment (n=2).
Reasons and practices for adherence
The explanatory model of the condition provides insight into how people conceive HIV infection, treatment, and adherence. These beliefs are complemented by the reasons for treatment adherence. Participants mentioned three main ones: maintaining good health (n=23), taking care of oneself for others (n=19), and staying alive (n=16).
Adherence is the maintenance of a series of practices in daily life. One type of practice focuses on the pharmacological aspect or medication use. The main practice is to incorporate in take into routine (n=22) either by associating it with specific times or actions, placing the medication in specific places, or carrying the medication. The patients mentioned the use of external reminders (n=18), such as notes, calendar, alarms, pillboxes, manually counting pills, and being reminded by people close to them as well as the internalization of medication intake (n=17), which is achieved when the person acquires a habit or “program” themselves, i.e., remembers to take the medication without requiring an external mechanism. Less frequently reported was the measure of resisting emotional discomfort (n=13), which includes self-motivation, thinking positively about the medication, or not discontinuing it even if they feel discomfort or are bored with the treatment.
One group of participants made reference to making their medication intake more flexible (n=11), which consists of actions such as not always taking the medication at the same time and not discontinuing it even if the time has passed or it has been forgotten at home. Some indicated a practice for the management of side effects (n=6) by anticipating them, changing the time or place where the medication is taken, as well as the medication.
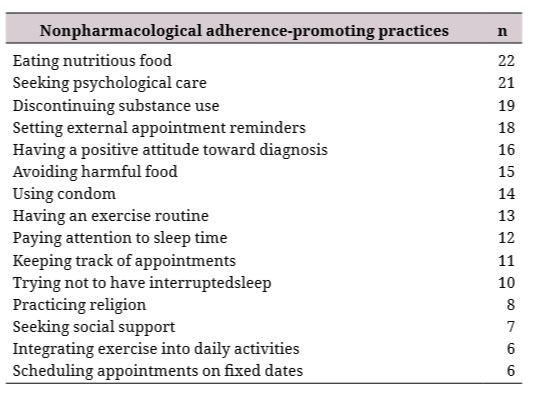
Although medication intake is a central aspect of treatment adherence for people living with HIV, this process is not limited to it. From an integral perspective, it is necessary to include a set of health care practices that make up the nonpharmacological aspect of the adherence process. Table 1 shows the core practices that complement medication intake. These practices are usually specific to different areas of care, such as nutrition, physical activity, rest, sexuality, mental health, avoidance of substance use, attendance at medical appointments, or laboratory studies.
Integration of the treatment adherence process
This section shows the relationships between the most relevant categories and subcategories. In the theoretical coding process, categories and subcategories were integrated to explain the process of treatment adherence in people living with HIV who attend CAPASITS in Tamaulipas, Mexico. This process proposes the link between explanatory models, motivations, and adherence-promoting practices.
To establish the relationships, one of the criteria was to use only the subcategories that appeared in at least 30 % of the cases. Subsequently, associations between the subcategories were identified by considering whether they appeared together in the same cases, i.e., based on their co-occurrence. To assess the degree of co-occurrence between subcategories, three levels were established—weak (co-occurrence in 30 %–39 % of cases), moderate (co-occurrence in 40 %–49 % of cases) and high (co-occurrence in ≥50 % of cases).
The categories and subcategories were organized in a visual map based on the following assumptions: explanatory models are constructed from certain sources of information and social relations, the explanatory model of the condition has an area linked to HIV infection and other areas linked to treatment and adherence, and the explanatory model builds the framework for making sense of pharmacological and nonpharmacological adherence-promoting practices and interacts with the motivations for adherence.
The most important source of information for the construction of the explanatory model was healthcare services. This model is composed of several areas. Regarding HIV infection, the participants consider that its main mechanism of action is affecting the immune system, which makes it essential for them to adopt a healthy lifestyle. With regard to antiretroviral therapy, its central function is to control the virus. Patients anticipate two consequences if treatment is not properly followed: deterioration of their health and the development of viral resistance. Within the explanatory model of the condition, they also construct a concept of adherence, which especially requires proper medication intake and being responsible for taking care of oneself. This means that becoming a patient has a moral implication and that adherence cannot be reduced to a “pharmaceuticalization” of daily life but entails a broader sense of care.
The explanatory model provides meaning to the process of adherence, but it is complemented by a set of motives. Although there are other motives such as staying alive and taking care of oneself for others, the main one is the maintenance of good health. Nonetheless, motives alone are not enough. Patients need to recognize that the condition involves adopting a healthy lifestyle, taking the medication, and being responsible for their well-being (Figure 2).

Note 1: Percentages represent the co-occurrence of subcategories across cases.
Note 2: The thickness of the lines on the maps represents the strength of the relationship between the subcategories according to their co-occurrence: weak (30 %–39 %), moderate (40 %–49 %), and strong (≥50 %).
Note 3: The framed subcategories are those considered central to the process owingto its degree of association with other subcategories and their relevance within the corresponding category.
The explanatory model of the condition and the development of reasons for adherence promote the implementation of a series of practices to facilitate medication intake. The main practice consists of linking medication intake with daily routine in addition to the use of external reminders or internalization of medication intake due to habit. The latter practice was named resisting emotional distress, which occurs especially after diagnosis, although not exclusively (Figure 3). These practices are most strongly linked to the reason of maintaining health, secondary to the motives of staying alive and taking care of oneself for others.

Note 1: Percentages represent the co-occurrence of subcategories across cases.
Note 2: The thickness of the lines on the maps represents the strength of the relationship between the subcategories according to their co-occurrence: weak (30 %–39 %), moderate (40 %–49 %), and strong (≥50 %).
Note 3: The framed subcategories are those considered central to the process owing to its degree of association with other subcategories and their relevance within the corresponding category.
The explanatory model of the condition and reasons for adherence facilitate the implementation of various nonpharmacological adherence practices focused on health care in a comprehensive manner that complements medication intake. Eating nutritious food and avoiding harmful ones was considered among the main practices. In addition to nutrition, mental health plays an important role in patient care as indicated by practices such as seeking psychological care and assuming a positive attitude toward the diagnosis. Other care practices are the use of a condom or cessation of substance use. With regard to medication intake, patients may resort to external reminders for medical appointments or laboratory studies (Figura 4). Nonpharmacological adherence practices were also linked mainly to the reason of maintaning good health and, to a lesser extent, the motives of staying alive and taking care of oneself for others.
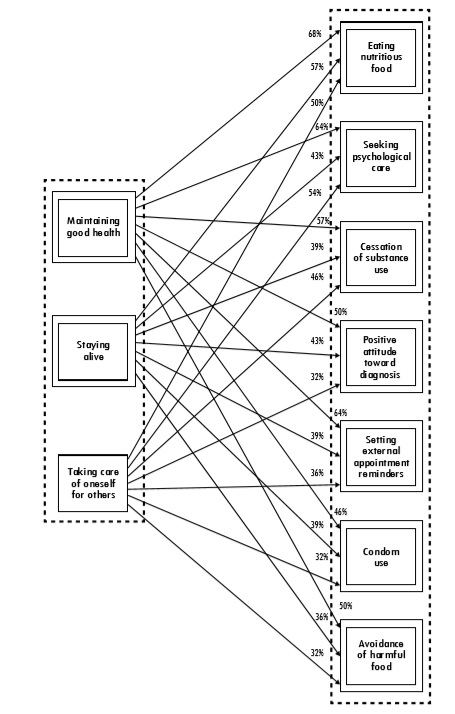
Note 1: Percentages represent the co-occurrence of subcategories across cases.
Note 2: The thickness of the lines on the maps represents the strength of the relationship between the subcategories according to their co-occurrence: weak (30 %–39 %), moderate (40 %–49 %), and strong (≥50 %).
Note 3: The framed subcategories are those considered central to the process owing to its degree of association with other subcategories and their relevance within the corresponding category.
Discussion
According to this study, treatment adherence in people living with HIV requires the continuous interaction of three main elements: the explanatory model of the condition, the reasons for continuing treatment, and a set of integrated healthcare practices. Adherence is conceived as a dynamic process that develops over time (18). At any point in time, patients may stop adhering to the treatment either intentionally or unintentionally since they maybe affected by personal and contextual barriers (19).
Healthcare services exert an important influence on the construction of the explanatory model on the condition since they are the main source of knowledge regarding HIV infection. However, patients develop a continued model, which retains a number of central notions. For example, they identify that HIV infection affects the immune system and antiretroviral therapy helps control virus replication. Previous studies have considered that knowledge regarding the condition is a functional competency that predicts adherence in people living with HIV (9).
One possible implication of this finding is that health education interventions may be beneficial to promote a minimal communication of these core notions since they provide a framework for justifying healthcare practices. Such interventions may also include information regarding side effects of the medication to promote informed treatment decision since the study revealed that patients particularly identified short-term side effects or only those that they had experienced themselves.
As a part of the explanatory model on treatment, patients anticipate the consequences of not following antiretroviral therapy, such as developing viral resistance and the deterioration of health. Previous studies have found that these beliefs about treatment facilitate adherence (7,20) and that they are maintained in the long term because patients receive feedback or evidence that their beliefs regarding treatment are correct by assessing the beneficial impact of care practices on their health status (10).
Patients construct representations of healthcare through communicative and intersubjective processes among the members of their social group, but such representations are in turn traversed by a continuous subjectification process where patients adopt the relevant elements for themselves (21). In this study, participants not only obtained the biomedical knowledge shared by the healthcare services to develop their explanatory model of the condition but also gave a new meaning to the condition favoring the process of adherence, such as associating it with a healthy lifestyle. This implies the acceptance of the biographical rupture generated by the condition and the need to generate a new way of living where HIV infection is integrated into everyday life.
The study suggests that explanatory models about the condition include the adherence aspec and that patients associate adherence with medication intake. It has been found that a single report of poor adherence may not be associated with immediate mortality, but it does increase the risk of recurrent poor adherence (5). Inasmuch as the loss of a few doses can lead to treatment failure, adherence levels of ≥95 % have been established although they may vary depending on the type of the antiretroviral drug (21).
Adherence was conceived by participants as the responsibility to take care of oneself. This coincides with the perspective of healthcare services where patients are considered as rational and intentional subjects who are assigned a greater responsibility for their care and have the ability to choose, without considering the differential limitations established by the social and economic structure (22).
Previous studies have identified an individual’s responsibility for adherence and commitment to the care of oneself as facilitators of adherence (23,24). Adherence is intimately linked to morality since it assumes that health depends not only on biological reasons but also on being able to exercise self-control, commit to comply with treatment, and be responsible not only in terms of care practices but also in terms of treatment outcomes. This requires that patients persist in continuous attention to their body and their way of life, both in health institutions and in intimate and personal living spaces (25).
The study revealed that the main reasons for adhering to treatment are maintaining good health and staying alive, which is consistent with that reported in previous studies (7,20,21,23,24,26). The treatment adherence model for people living with HIV also found that motives such as maintenance of health and being cared for by people who are close to them favor medication intake (8). These types of motives are expressed by adherent patients who accept the influence of HIV infection on their lives and are also characterized by experiencing treatment as their own decision, being informed about treatment, incorporating it into their daily routine, being open to social support, and proactively managing medication demands (11). The main practices promoting pharmacological adherence prevent the development of short-term nonadherence patterns, such as missing medication for an entire day, missing doses, taking medication several hours late or not following the dietary or drink requirements of medication intake (19). The main practices were the adjustment of medication intake to a daily routine (6,7,20,23,24,26), the use of external reminders (6,23,24), and the internalization of medication intake, which is achieved by repeating the medication intake routine for a long time, creating a habit, and generating automatic contextual cues that maintain the behavior (10).
To a lesser extent, patients mentioned the strategy of mood management (27), which is required in the presence of emotional distress which may arise especially after diagnosis or in the face of health crises during the course of infection. Emotional distress is linked to longterm nonadherence patterns, such as rarely taking the medication or alternating between extended periods of taking and not taking the medication (19).
Previous literature has focused primarily on practices that facilitate medication intake, also referred to as pharmacological adherence. However, they have not approached the study of adherence from a comprehensive perspective, which incorporates the nonpharmacological aspect wherein healthcare practices in multiple areas are grouped. Some studies report links between nonpharmacological adherence and variables such as age (28). In this study, the most relevant practices were maintaining a nutritious diet, attending psychological care, adopting a positive attitude toward the diagnosis, using reminders to attend appointments, reducing substance abuse, and using condoms.
In healthcare services, care is based on the logic of “conscious choice of actions” for the control of a biological disease. However, patients use a practical logic of care that is not always expressed consciously and is associated with other aspects of life. In the daily lives of patients, medical recommendations intersect with personal tastes, contextual possibilities, and moments of life (29). Difficulties may arise in the patient–healthcare services relationship, when the treatment prescription does not recognize the patient as a desiring being who has the right to build alternative life projects (30).
In the study, participants expressed difficulties in abandoning certain practices such as substance use (26,31), eating harmful food, or not using condoms. Because they contradict treatment prescriptions, patients often do not communicate these issues to healthcare personnel and do not access services available for their management, leading to the possibility of future health risks.
Considering the person with HIV as a central agent in their health care, this study shows that in patients attending specialized public services in the state of Tamaulipas, the explanatory model and motives shape adherence-promoting practices from an integral perspective. Future studies need to complement this perspective centered in the individual by exploring the role of relationships with healthcare services and the institutional context in promoting adherence. This is because although it has been found that satisfaction with the information received in healthcare services is not associated with pharmacological adherence (32), it is necessary to analyze how the intersection between information, gender, social class, and ethnicity can affect the adherence process.
The same applies for stigma since previous studies have revealed a relationship between stigma and adherence, and evaluating differences according to gender showed that men are affected to a greater extent (33). Therefore, gender-sensitive interventions are recommended to reduce stigma. Although the study included women, homosexual men as well as heterosexual men from different geographic areas of the state, one limitation is that the perspective of other groups of people living with HIV needs to be taken into account. In addition, patients reporting high levels of adherence or presenting undetectable viral load predominated. In future studies it will be important to establish comparisons between patients with different levels of adherence and at different clinical stages.
This study proposes that for promoting adherence, understanding the patient’s explanatory model with regard to the elements of condition, treatment, and adherence is required. The construction of explanatory models that facilitate adherence can be achieved through multiple interventions, such as psychoeducational interventions, a direct communication with the patient, through adherence clubs, and dissemination of information through printed or digital media. Interventions that allow communication with healthcare personnel via mobile telephony have enabled viral suppression in nonadherent patients at levels similar to traditional care (34).
However, mere knowledge about the condition is not enough; the patient should have motives that can sustain care over time. It is therefore important to assess the degree to which the patient takes care of themself in order to maintain their health since this implies a greater commitment and internal control. Some patients may benefit from external motivations such as the need to care for others. Preventing difficulties in the adherence process may be aided by assessing the reasons and identifying mental health problems that may limit the commitment to self-care. It has been found that early detection is not enough. Moreover, there are limitations to continue treatment after referral to psychological or psychiatric care services; however, there is greater viability in interventions based on peer support (35).
In case of nonadherent patients with mental health and/or treatment motivation problems, psychosocial interventions, such as individual counseling, support groups, and family-centered services and networks, are required to facilitate treatment retention (36). When providing care to the most vulnerable groups, group interventions should not only promote adherence but also reduce the stigma and their mistrust of healthcare personnel (37).
Finally, the practice of medication intake would be facilitated by behavioral interventions such as the use of external reminders and the incorporation of medication intake into the daily routine, within the framework of a continuously assessed adherence process. Interventions using smart pill dispensers that transmit real-time data on adherence and send telephone or text messages to nonadherent patients for facilitating medication intake are promising (38), especially at the start of treatment. Furthermore, pharmacological adherence suggests a personalized evaluation of the various areas of care in order to channel the corresponding specialists for detecting difficulties. In this sense, approaching adherence from a comprehensive perspective implies multidisciplinary work, continuous assessment, and personalized interventions taking into account the resources of each patient and the contextual barriers that may affect their care process.
Authorship statement
The authors declare that each one has contributed in all the stages of the research: conceptualization, methodology, investigation, formal analysis, writing the original draft, reviewing and editing.
Conflict of interests
None declared.
Disclaimer
This work was possible because of the funding granted by the Program for the Professional Development of Teachers (PRODEP) for the project “Strategies and barriers for therapeutic adherence in people living with HIV in the state of Tamaulipas,” with the official number of the release letter being DSA/103.5/15/7318.
References
1. Chesney M, Morin M, Sherr L. Adherence to HIV combination therapy. Soc Sci Med. 2000;50(11):1599-605. https://doi.org/10.1016/s0277-9536(99)00468-2
2. Pound P, Britten N, Morgan M, Yardley L, Pope C, Daker-White G, et al. Resisting medicines: a synthesis of qualitative studies of medicine taking. Soc Sci Med. 2005;61:133-55. https://doi.org/10.1016/j.socscimed.2004.11.063
3. Vilató L, Martin L, Pérez, I. Adherencia terapéutica y apoyo social percibido en personas que viven con VIH/Sida. Rev Cub Public Health. 2015;41(4):620-30.
4. Menéndez E. Modelo hegemónico, modelo alternativo subordinado, modelo de autoatención. Caracteres estructurales. In: Campor R, editor. La antropología médica en México. Mexico City: Mora Institute; 1992. p. 97-114.
5. Kiwuwa-Muyingo S, Oja H, Walker A, Ilmonen P, Levin J, Mambule I, et al. Dynamic logistic regression model and population attributable fraction to investigate the association between adherence, missed visits and mortality: a study of HIV-infected adults surviving the first year of ART. BMC Infect Dis. 2013;13(1):395. https://doi.org/10.1186/1471-2334-13-395
6. Bezabhe W, Chalmers L, Bereznicki L, Peterson G, Bimirew M, Kassie D. Barriers and facilitators of adherence to antiretroviral drug therapy and retention in care among adultHIV-positive patients: a qualitative study from Ethiopia. Plos One. 2014;9(5):e97353. https://doi.org/10.1371/journal.pone.0097353
7. Krummenacher I, Spencer B, Du Pasquier S, Bugnon O, Cavassini M, Schneider M. Qualitative analysis of barriers and facilitators encountered by HIV patients in an ART adherence programme. Int J Clin Pharm. 2014;36(4):716-24. https://doi.org/10.1007/s11096-014-9930-0
8. Kennedy S, Goggin K, Nollen N. Adherence to HIV medications: utility of the theory of self-determination. Cognit Ther Res. 2004;28(5):611-28. https://doi.org/10.1023/B:COTR.0000045568.95219.e2
9. Sánchez-Sosa J, Cázares O, Piña J, Dávila M. Un modelo psicológico en los comportamientos de adhesión terapéutica en personas con VIH. Mental Health. 2009;32(5):389-97
10. Phillips A, Leventhal H, Leventhal E. Assessing theoretical predictors of long-term medication adherence: patient´s treatment-related beliefs, experiential feedback and habit development. Psychol Health. 2013;28(10):1135-51. https://doi.org/10.1080/08870446.2013.793798
11. Vervoort S, Grypdonck M, de Grauwe A, Hoepelman A, Borleffs J. Adherence to HAART: processes explaining adherence behavior in acceptors and non-acceptors. AIDS Care. 2009;21(4):431-8. https://doi.org/10.1080/09540120802290381
12. Kleinman A. Patients and healers in the context of culture. An exploration of the borderland between Anthropology, Medicine, and Psychiatry. Berkeley: University of California Press; 1980.
13. Centro Nacional para la Prevención y Control del VIH y el Sida. Vigilancia epidemiológica de casos de VIH/sida en México. Registro Nacional de Casos de SIDA 2018 [Internet]. Mexico: Censida; 2019. [Cited 2019 Jun 17]. Available from: https://www.gob.mx/censida/documentos/epidemiologia-registro-nacional-de-casos-de-sida?idiom=es
14. Peñarrieta M, Kendall T, Martínez N, Rivera A, Gonzales N, Flores F, et al. Adherencia al tratamiento antirretroviral en personas con VIH en Tamaulipas, Mexico. Rev Peru Med Exp Public Health. 2009;26(3):333-7.
15. González M, Ybarra J, Piña J. Relaciones sociales, variables psicológicas y conductas de adherencia en adultos con VIH. Rev Int Psicol Ter Psicol. 2012;12(2):173-84.
16. Balandrán D, Gutiérrez J, Romero M. Evaluación de la adherencia antirretroviral en México: adherencia de cuatro días vs índice de adherencia. Rev Invest Clin. 2013;65(5):38491.
17. Charmaz K. Constructing grounded theorya: a practical guide through qualitative analysis. California: Sage; 2006.
18. Spire B, Duran S, Souville M, Leport C, Raffi F, Moatti JP, et al. Adherence to highly active antiretroviral therapies (HAART) in HIV-infected patients: from a predictive to a dynamic approach. Soc Sci Med. 2002;54(10):1481-96. https://doi.org/10.1016/s0277-9536(01)00125-3
19. Hill Z, Kendall C, Fernandez M. Patterns of adherence to antiretrovirals: why adherence has no simple measure. AIDS Patient Care STDs. 2003;17(10):519-25. https://doi.org/10.1089/108729103322494311
20. Sidat M, Fairley C, Grierson J. Experiences and perceptions of patients with 100 % ad- herence to highly active antiretroviral therapy: a qualitative study. AIDS Patient Care STDs. 2007;21(7):509-20. https://doi.org/10.1089/apc.2006.0201
21. Muñoz N. Reflexiones sobre el cuidado de sí como categoría de análisis en salud. Salud Colect. 2009;5(3):391-401.
22. Menéndez E. De sujetos, saberes y estructuras: introducción al enfoque relacional en el estudio de la salud colectiva. Buenos Aires: Lugar Editorial; 2009.
23. Brion J, Menke E. Perspectives regarding adherence to prescribed treatment in highly adherent HIV-infected gay men. J Assoc Nurses AIDS Care. 2008;19(3):181-91. https://doi.org/10.1016/j.jana.2007.11.006
24. Lewis M, Colbert A, Erlen J, Meyers M. A qualitative study of persons who are 100 % adherent to antiretroviral therapy. AIDS Care. 2006;18(2):140-8. https://doi.org/10.1080/09540120500161835
25. Del Monaco R. Autocuidado, adherencia e incertidumbre: tratamientos biomédicos y experiencias de pacientes en el dolor crónico de la migraña. Salud Colect. 2013;9(1):65-78.
26. Castro E, Santiago L, Jiménez J, Dávila-Vargas D, Rosal M. A social-ecological view of barriers and facilitators for HIV treatment adherence: interviews with Puerto Rican HIV patients. PLoS One. 2015;10(9):e0125582. https://doi.org/10.1371/journal.pone.0125582
27. Malcolm S, Ng J, Rosen R, Stone V. An examination of HIV/AIDS patients who have excellent adherence to HAART. AIDS Care. 2003;15(2):251-61. https://doi.org/10.1080/0954012031000068399
28. Varela T, Hoyos P. La adherencia al tratamiento para el VIH-SIDA: más allá de la toma de antirretrovirales. Rev Salud Pública. 2015;17(4):528-40. https://doi.org/10.15446/rsap.v17n4.38429
29. Domínguez A. Los cuidados de la salud en personas que viven con diabetes: enfoque etnográfico antropológico y perspectiva de género. Salud Colect. 2017;13(3):375-90. https://doi.org/10.18294/sc.2017.1156
30. Seixas C, Merhy E, Baduy R, Junior H. La integralidad desde la perspectiva del cuidado en salud: una experiencia del Sistema Único de Salud en Brasil. Salud Colect. 2016;12(1):11323. https://doi.org/10.18294/sc.2016.874
31. Panos S, Del Re A, Thames A, Arentsen T, Patel S, Castellon S, et al. The impact of neurobehavioral features on medication adherence in HIV: evidence from longitudinal models. AIDS Care. 2014;26(1):79-86. https://doi.org/10.1080/09540121.2013.802275
32. Pacífico J, Gutiérrez C. Información sobre la medicación y adherencia al tratamiento antirretroviral de gran actividad en pacientes con VIH/SIDA de un hospital de Lima, Perú. Rev Peru Med Exp Salud Publica. 2015;32(1):66-72.
33. Zafra-Tanaka JH, Ticona-Chavez E. Estigma relacionado a VIH/SIDA asociado con adherencia al tratamiento antirretroviral en pacientes de un hospital de Lima, Perú 2014. Rev Peru Med Exp Salud Publica. 2016;33(4):625-32. https://doi.org/10.17843/rpmesp.2016.334.2544
34. Ventuneac A, Kaplan-Lewis E, Buck J, Roy R, Aberg CE, Duah BA, et al. A mobile health intervention in HIV primary care: supporting patients at risk for ART non-adherence. HIV Res Clin Pract. 2020;21(5):140-50. https://doi.org/10.1080/25787489.2020.1862972
35. Been SK, van de Vijver DAMC, Smit J, Bassant N, Pogány K, Stutterheim SE, et al. Feasibility of four interventions to improve treatment adherence in migrants living with HIV in the Netherlands. Diagnostics (Basel). 2020;10(11):980. https://doi.org/10.3390/diagnos-tics10110980
36. Okonji EF, Mukumbang FC, Orth Z, Vickerman-Delport SA, Van Wyk B. Psychosocial support interventions for improved adherence and retention in ART care for young people living with HIV (10–24 years): a scoping review. BMC Public Health. 2020;20:1841. https://doi.org/10.1186/s12889-020-09717-y
37. Bogart LM, Barreras JL, Gonzalez A, Klein DJ, Marsh T, Agniel D, et al. Pilot randomized controlled trial of an intervention to improve coping with intersectional stigma and medication adherence among HIV-positive latinx sexual minority men. AIDS Behav. 2021;25:1647-60. https://doi.org/10.1007/s10461-020-03081-z
38. Ellsworth GB, Burke LA, Wells MT, Mishra S, Caffrey M, Liddle D, et al. Randomized pilot study of an advanced smart-pill bottle as an adherence intervention in patients with HIV on antiretroviral treatment. J Acquir Immune Defic Syndr. 2021;86(1):73-80. https://doi.org/10.1097/QAI.0000000000002519
Notes
Acknowledgment We thank the users and health personnel of CAPASITS of the State of Tamaulipas who collaborated in carrying out the study.
Author notes
* Corresponding author: agomez82@uabc.edu.mx