

Evaluation of Differences in Metabolic and Immunologic Markers and Cardiovascular Risk in hiv-1 Patients
Evaluación de la relación entre marcadores metabólicos, inmunológicos y de riesgo cardiovascular en pacientes con vih-1
Avaliação da relação entre marcadores metabólicos, imunológicos e de risco cardiovascular em pacientes com hiv-1
Evaluation of Differences in Metabolic and Immunologic Markers and Cardiovascular Risk in hiv-1 Patients
Revista Ciencias de la Salud, vol. 19, no. 3, 2021
Universidad del Rosario
Received: 19 may 2020
Accepted: 20 April 2021
Additional information
To cite this article: Castro G, León K, Marín-Palma D, Oyuela SM, Cataño-Bedoya J-U, Duque-Botero J, Giraldo-Méndez DP, Taborda NA, Hernández JC, Rugeles MT, Jaimes FA. Evaluation of Differences in Metabolic and Immunologic Markers and Cardiovascular Risk in HIV-1 Patients Rev Cienc Salud. 2021;19(3):1-18. https://doi.org/10.12804/revistas.urosario.edu.co/revsalud/a.10532
Abstract: Introduction: hiv infection induces an exacerbated chronic inflammatory response, which triggers metabolic disorders and cardiovascular diseases; however, there are individuals, known as hiv controllers, who do not have typical progression markers. As cardiovascular risk tests are not accurate on hiv-1 infected patients, the study of metabolic and inflammatory parameters in individuals with different patterns of progression could contribute to the definition of predictors of cardiovascular disease in this population. The aim of this study was to compare hiv controllers and hiv progressors (with and without antiretroviral therapy) as well as with healthy controls in order to explore differences and correlations in metabolic and inflammatory biomarkers associated with cardiovascular risk. Materials and methods: This was a cross-sectional analytical study which included 63 individuals infected with hiv-1 classified as hiv controllers or progressors (with or without antiretroviral therapy), and a healthy control group. The following parameters were determined: carotid intima-media thickness (cimt); cardiovascular risk scores; lipid profile, fasting glucose, high-sensitivity crp, D-dimer, sCD14, sCD163, il-6, and il-18. Data were compared with Anova or Kruskal–Wallis, and correlations were evaluated by the Spearman coefficient. Results:While there were no significant differences in Framingham, dad or cimt values, hiv controllers exhibited lower triglycerides levels when compared with hiv progressors. No differences were observed in markers, such as high-sensitivity crp, il-6, il-18, and sCD163, among the groups. The median hdl value was higher in hiv progressors on antiretroviral therapy, and cimt in hiv controllers was negatively correlated with sCD14. Conclusion: hiv controllers have a different cardiovascular profile than hiv progressors according to their values in metabolic and immunological biomarkers.
Keywords: hiv-1, cardiovascular diseases, inflammation, disease progression.
Resumen: Introducción: la infección por vih-1 induce una respuesta inflamatoria crónica exacerbada que desencadena alteraciones metabólicas y cardiovasculares; sin embargo, algunos individuos “controladores” no presentan los marcadores de progresión típicos. Dado que las pruebas que evaluan el riesgo cardiovascular carecen de precisión en pacientes con vih-1, el estudio de parámetros inflamatorios en individuos con diferente progresión podría aportar a la definición de predictores de enfermedad cardiovascular en esta población. El objetivo es explorar diferencias y correlaciones en biomarcadores metabólicos e inflamatorios asociados con riesgo cardiovascular, comparando individuos controladores y progresores con y sin terapia antiviral. Materiales y métodos: estudio analítico transversal con 63 individuos infectados por vih-1, clasificados en controladores y progresores (con terapia antiviral y sin esta), y controles sanos. Se midió el grosor de la íntima media carotidea (cimt), puntajes de riesgo cardiovascular y cuantificación de perfil lipídico, glucemia en ayunas, pcr ultrasensible, dímero D, sCD14, sCD163, il-6 e il-18. Se realizó comparación por Anova o Kruskal-Wallis y correlación por coeficiente de Spearman. Resultados: no hubo diferencias significativas en índices de Framingham, dad o cimt, pero los individuos controladores presentaron menores valores de triglicéridos, comparados con los progresores. No se observaron diferencias en pcr ultrasensible, il-6, il-18, y sCD163, entre los grupos estudiados. La mediana del hdl fue mayor en los progresores con terapia antiviral y el cimt en los controladores se correlacionó negativamente con sCD14. Conclusión: los individuos controladores presentan un perfil cardiovascular diferente a los individuos progresores, de acuerdo con los biomarcadores metabólicos e inmunológicos evaluados.
Palabras clave: vih-1, enfermedades cardiovasculares, inflamación, progresión de la enfermedad.
Resumo: Introdução: a infecção pelo hiv-1 induz resposta inflamatória crônica exacerbada, que desencadeia alterações metabólicas e doenças cardiovasculares; no entanto, existem indivíduos, chamados controladores, que não possuem os marcadores de progressão típicos. Tendo em vista que os testes que avaliam o risco cardiovascular carecem de precisão em pacientes com hiv-1, o estudo de parâmetros metabólicos e inflamatórios em indivíduos com diferentes padrões de progressão pode contribuir para a definição de preditores de doença cardiovascular nessa população. O objetivo é explorar diferenças e correlações em biomarcadores metabólicos e inflamatórios associados ao risco cardiovascular, comparando indivíduos controladores e progressores submetidos ou não à terapia antiviral. Materiais e métodos: Estudo analítico transversal que incluiu 63 indivíduos infectados pelo hiv-1, classificados como controladores e progressores (com e sem terapia antiviral), além de grupos controle saudáveis. Realizou-se a medição da espessura da íntima média da carótida (cimt), pontuações de risco cardiovascular; e quantificação do perfil lipídico, glicemia em jejum, pcr ultrassensível, dímero D, sCD14, sCD163, il-6 e il-18. A comparação foi feita por Anova ou teste de Kruskal-Wallis e a correlação pelo coeficiente de Spearman. Resultados. Embora não tenha havido diferenças significativas nos índices de Framingham, dad ou cimt, os indivíduos controladores apresentaram valores de triglicerídeos mais baixos, em comparação com os progressores. Não foram observadas diferenças em marcadores como pcr ultrassensível, il-6, il-18 e sCD163, entre os grupos estudados. O hdl médio foi maior em indivíduos progressores em terapia antiviral, e o cimt em indivíduos controladores foi negativamente correlacionado com o sCD14. Conclusão: os indivíduos controladores apresentam um perfil cardiovascular diferente dos indivíduos progressores, de acordo com os biomarcadores metabólicos e imunológicos avaliados.
Palavras-chave: hiv-1, doenças cardiovasculares, inflamação, progressão da doença.
Introduction
Although highly active antiretroviral therapy (haart) has increased survival and improved the quality of life of patients with hiv-1 (human immunodeficiency virus type 1), the emergence of other diseases, caused by the chronic effects of this infection or as a consequence of the adverse events of antiretroviral drugs, has increased in this population (1). Reports indicate that 49% of the deaths of patients with hiv-1 infection are due to events associated with Acquired Immunodeficiency Syndrome (aids), 7% due to liver diseases, and 6.5% due to cardiovascular diseases (cvd) (2,3). Alarmingly, mortality due to cvd among patients with hiv-1 has increased, mainly as a result of myocardial infarction, sudden death, and stroke (4).
Cardiovascular risk has been associated with chronic inflammatory state characteristic of hiv-1 infection, where the amount of proteins, such as il-6, high-sensitivity crp (C-reactive protein), D-dimer, sCD163, sCD14, and il-18, among others, is increased (5). In addition, immune activation and prolonged treatment with antiretrovirals, especially protease inhibitors (6,7), trigger metabolic alterations in patients with hiv-1. These metabolic alterations cause elevations of low-density lipoproteins (ldl) and triglycerides along with a reduction in high-density lipoproteins (hdl) (8), which together enhance cardiovascular risk (9,10).
There are several strategies for estimation of cardiovascular risk, including the Framingham atp iii scores and dad (Data Collection on Adverse Events of Anti-hiv Drugs Study) (11), as well as complementary studies, such as the carotid intima-media thickness (cimt) test (12). Although these tests show good accuracy in the general population (13), their use in patients with hiv-1 is debated given the complexity of this infection and the variation in clinical evolution among patients.
There are patients capable of spontaneously controlling viral replication, called elite or viremic controllers, who have undetectable viral loads or viral load less than 2000 copies/ mL, respectively, despite having at least one year of diagnosis of the infection in the absence of haart (14,15). These patients have been the subject of multiple investigations aimed at identifying the immunogenetic mechanisms associated with viral control (15). Evidence indicates that most of the immunological parameters of hiv controller individuals remain similar to those of uninfected individuals and that their immune system cells have a high functional capacity (16,17). However, there are still limited studies assessing the clinical characteristics related to cardiovascular risk, such as cimt, in these patients with a particular evolution of hiv-1 infection. Consequently, given the existence of different phenotypes of infection progression and difficulties in determining cardiovascular risk in patients with hiv-1, this study aimed to explore the differences and correlations between metabolic and inflammatory markers in individuals with different patterns of progression, and whether the metabolic and inflammatory markers could be use for defining parameters that complement the assessment of cardiovascular risk in these patients.
Materials and methods
This was a cross-sectional analytical study, which included patients of both sexes over 18 years old and with confirmed diagnosis of hiv-1 infection, recruited between 2016 and 2017 in two health service institutions in Medellin, Colombia. The study included individuals with hiv-1 classified into the following groups: i) Controllers, defined as patients with more than one year of diagnosis and a viral load less than 2,000 copies/mL in the absence of haart; ii) progressors (defined as patients who presented clinical, immune or virological deterioration characterized by a history of cd4+ T lymphocyte counts <500 cells/uL and viral loads >2000 copies/mL) with haart, or iii) progressors patients without haart. Additionally, a control group was included comprising individuals who were hiv-1 negative. Exclusion criteria included patients with a previous history of cardiovascular events or diabetes; patients with virologic failure, active opportunistic disease or under immunosuppressive treatment; pregnant or breastfeeding women; patients with active neoplasia and patients under treatment with statins.
Current national and international standards for data management and confidentiality were considered. The ethical principles of the Declaration of Helsinki, Belmont Report, and cioms Guidelines were followed, taking into account the principle of proportionality between predictable risks and possible benefits. An informed consent form was developed and filled out for each patient, which was previously approved by the Bioethics Committee of the University Research Center of Universidad de Antioquia (record no. 15-08-636) and the Bioethics Subcommittee of Unversidad Cooperativa de Colombia, Medellin Campus (record no. 0800-015).
Given the low frequency of hiv controllers and the changes in the clinical management of patients with hiv-1, who receive antiretroviral therapy in the initial months of diagnosis regardless of their clinical parameters, this study included 63 patients with hiv-1through convenience sampling, who were distributed into 13 controllers, 31 hiv progressors with haart, and 19 hiv progressors without haart. A group of 10 healthy controls was included to validate baseline values for the variables used.
The cimt was measured at Hospital San Vicente Fundación, using a color Doppler echocardiography with high-resolution B-mode ultrasound with pulsed Doppler (General Electric, logiq F8, usa). The Framingham and dad scores (cardiovascular risk predictors) were determined by means of algorithms designed and validated in various populations, including Colombian populations, using public calculators for this purpose (18-20). The variables necessary to calculate these values were obtained through a demographic and clinical survey, in which data were collected on sex, body mass index, age, systolic blood pressure, smoking (current or previous), family history of cvd, diabetes, exposure to antiretrovirals, as well as duration of antriretroviral therapy. cimt was measured by vascular physicians from the Hospital San Vicente Fundación, and donor assessment and data collection were performed by a clinical epidemiologist with a Master’s degree in hiv.
Approximately 4 mL of peripheral blood was collected via venipuncture in a Vacutainer tube with edta, 4 mL of anticoagulated blood with heparin in a Vacutainer tube, and 18 mL of blood in a Vacutainer tube without anticoagulant. Plasma and serum were obtained from the blood sample through centrifugation and stored at −70 °C until being processed.
Glycemia (uv hexokinase test), high-sensitivity crp (immunoturbidimetry), and D-dimer (immunochromatography) values were quantified in a validated laboratory in Medellin, Colombia. These tests were performed on peripheral blood collected via venipuncture in Vacutainer tubes with anticoagulant heparin and tubes without anticoagulant, which were transported to the laboratory under stringent measures.
Serum levels of hdl, total cholesterol and triglycerides were quantified by colorimetric assay using a commercial kit (Biosystems; Costa Brava 30, Barcelona, Spain) (21). Results were reported in mg/dL.
The following methodology was employed for performing cd4+ T lymphocyte counts: i) Differential white cell count by Wright’s stain; ii) total white cell count and iii) T lymphocyte count using monoclonal antibodies specific for cd3 (Anti-cd3-fitc; clone: ucht1), cd4 (Anti-cd4- apc; clone: rpa-T4) and cd8 (Anti-cd8-pe, clone: rpa-T8) (eBioscience, San Diego, usa) by Flow cytometry (facs bd Biosciences, San Jose, ca, usa). Plasma viral load for hiv-1 was determined by a certified clinical laboratory, using the commercial Ampliprep-Cobas Amplicor rt-pcr assay (Roche, Indianapolis, in; detection limit 20 copies/mL) on peripheral blood samples collected via venipuncture in tubes with the anticoagulant, edta.
Quantification of soluble markers was performed by enzyme-linked immunosorbent assays. The commercial kit Human Soluble Cluster of Differentiation 14 (cd14)- mbs2514176_coa (MyBioSource, San Diego, usa) was used for detection of sCD14 factor. The commercial kit Human sCD163 Ready-SET-Go 88-50360-22 (Affymetrix eBioscience, Vienna, Austria) was used for detection of sCD163. The Human il-18 Matched Antibody Pairs BMS267/2MSTkit (eBioscience, Vienna, Austria) was used for detection of il-18, and the bd OptEIAcommercial kit (bd Biosciences) was used for detection of il-6. All assays were performed in duplicate and according to the manufacturer’s instructions, and the reading was done using the Multiskan Thermo Fisher, fc Microplate Photometer (Waltham, usa).
Data distribution of the quantitative variables was determined based on the Shapiro- Wilk test. Accordingly, analysis of variance (Anova) or Kruskal–Wallis tests were applied for parametric or nonparametric data, respectively. In addition, a Dunn’s post hoc test was applied. Correlations were estimated by Pearson or Spearman linear correlation analysis, according to the normality test. All analyses were performed by subgroups, according to the progression profile and haart being used or not. Data were stored and analyzed in Statistical Package for the Social Sciences version 22.0 (Armonk, ny, usa). In all analyses, a value of p < 0.05 was considered statistically significant.
The selection of participants was controlled by strict compliance with the inclusion and exclusion criteria, as well as by checking their clinical history and repeating laboratory tests, if necessary. Recall bias regarding classification, time of diagnosis, and previous treatment with haart was controlled by reviewing the patient’s clinical history. Laboratory procedures were performed in a blind manner, with a clearly defined protocol and with a previous standardization process. Surveys were carried out by personnel trained to fill out and take the indicated measurements. For the collection of information, data was entered twice, and a backup copy of the information was kept.
Results
Patient registration and main characteristics of the participants are summarized in Figure 1 and Table 1. It should be emphasized that the median time to diagnosis was 28 months (iqr 22–50) for controllers, 16 months (iqr 2–40) for non-haart hiv progressors and 78 months (iqr 35–126) for haart hiv progressors. All haart hiv progressors were treated with nucleoside/nucleotide reverse transcriptase inhibitors; 54% of them were also taking non-nucleoside reverse transcriptase inhibitors; 16.4% were receiving protease inhibitors, and 1.4% integrase in-hibitors. Finally, 46%, 63%, 55%, and 30% of the controllers, non-haart hiv progressors, haart hiv progressors and healthy controls were men, respectively. Regarding active smoking, 15%, 32%, 29%, and 10% of each group, respectively, were smokers.
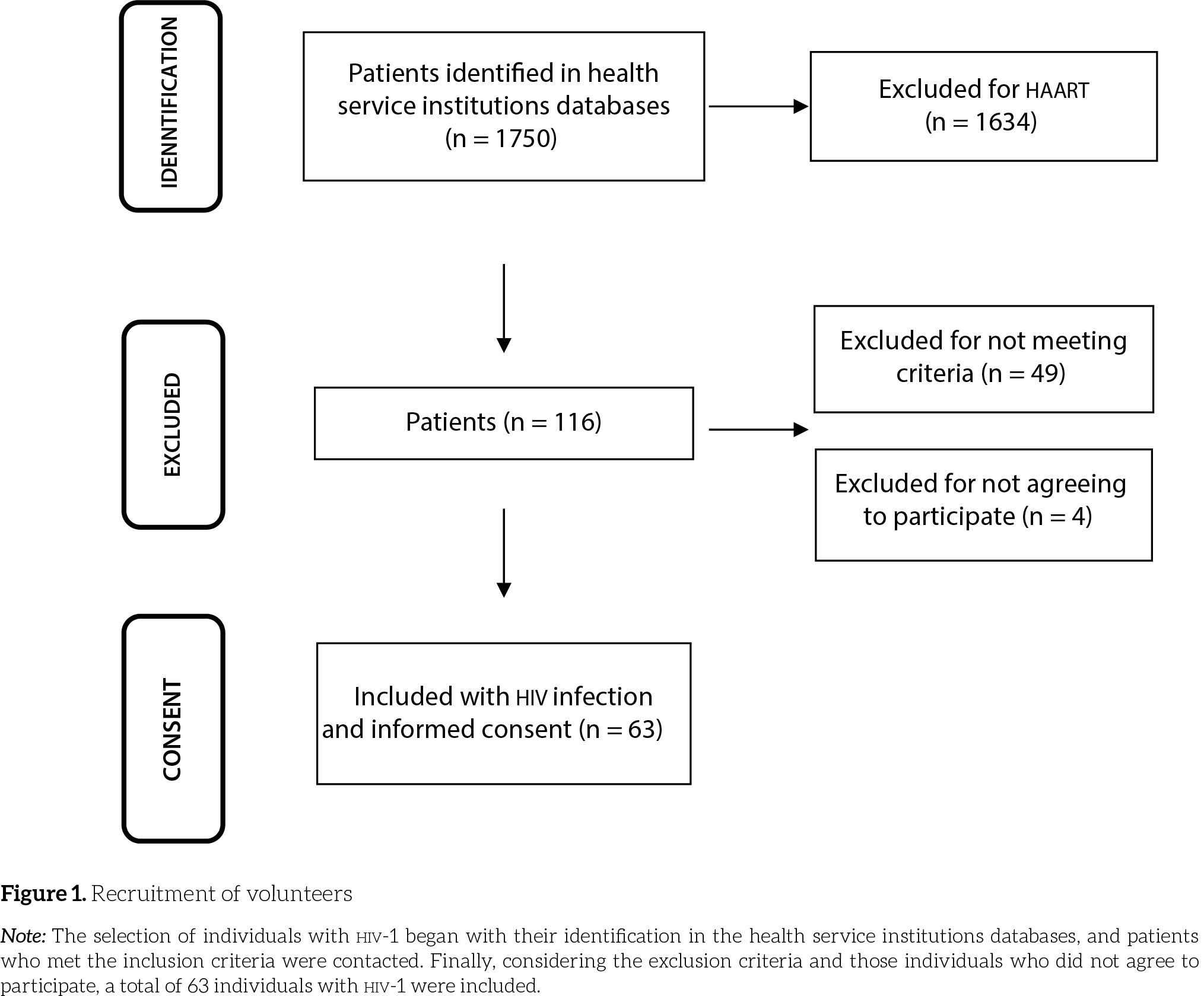
Note: The selection of individuals with hiv-1 began with their identification in the health service institutions databases, and patients who met the inclusion criteria were contacted. Finally, considering the exclusion criteria and those individuals who did not agree to participate, a total of 63 individuals with hiv-1 were included.

No statistically significant differences were found between the medians of the hiv controller and progressor groups with or without haart in the Framingham score (p = 0.911) or the dad score (p = 0.213). When assessing cimt thickness as a predictor of cardiovascular risk, no significant differences were observed among different groups either (p = 0.856) (Table 2).


Individuals with hiv-1 had different hdl levels, with progressors presenting lower levels, followed by hiv controllers and haart hiv progressors (p < 0.0001; Figure 2A). It is important to highlight that in general, infected individuals presented lower hdl levels than healthy controls (Figure 2A). In contrast, individuals with hiv-1 showed higher levels of triglycerides compared to healthy controls, being higher in non-haart progressors (p = 0.005; Figure 2B). As for total cholesterol (p = 0.089) and ldl (p = 0.318) levels, no significant differences were observed between the groups of infected patients, nor in comparison with healthy controls (Table 2).

Note: In serum from individuals with hiv-1 and healthy controls, (A) hdl (B) Triglycerides and (C) Fasting glycemia were quantified. Statistical comparisons were performed using the Kruskal–Wallis test with a 95% confidence interval and a Dunn’s hoc post-test was applied. Significant differences are shown at the top of the figures (* p < 0.05; ** p < 0.01; *** p < 0.0001).
Although no difference was found in fasting glycemia between the groups of patients with infection (p = 0.091), median glycemia of healthy controls was observed to be lower than that of individuals with hiv-1, particularly with respect to hiv progressors under therapy. No significant differences were observed in high-sensitivity crp and D-dimer levels among individuals with the virus (p = 0.754 and p = 0.115, respectively) (Table 2). There were also no significant differences in il-6, il-18, sCD14, or sCD163 levels among study individuals (Table 2).
We evaluated whether Framingham, dad scores, and cimt were related to the different soluble inflammatory markers. In this case, a statistically significant negative correlation was detected between sCD14 and cimt values (rho = −0.712, p = 0.006) in hiv controllers. Regarding the other variables (high-sensitivity crp, D-dimer, il-6, il-18, and cd163s) no significant correlations were found (Table 3).
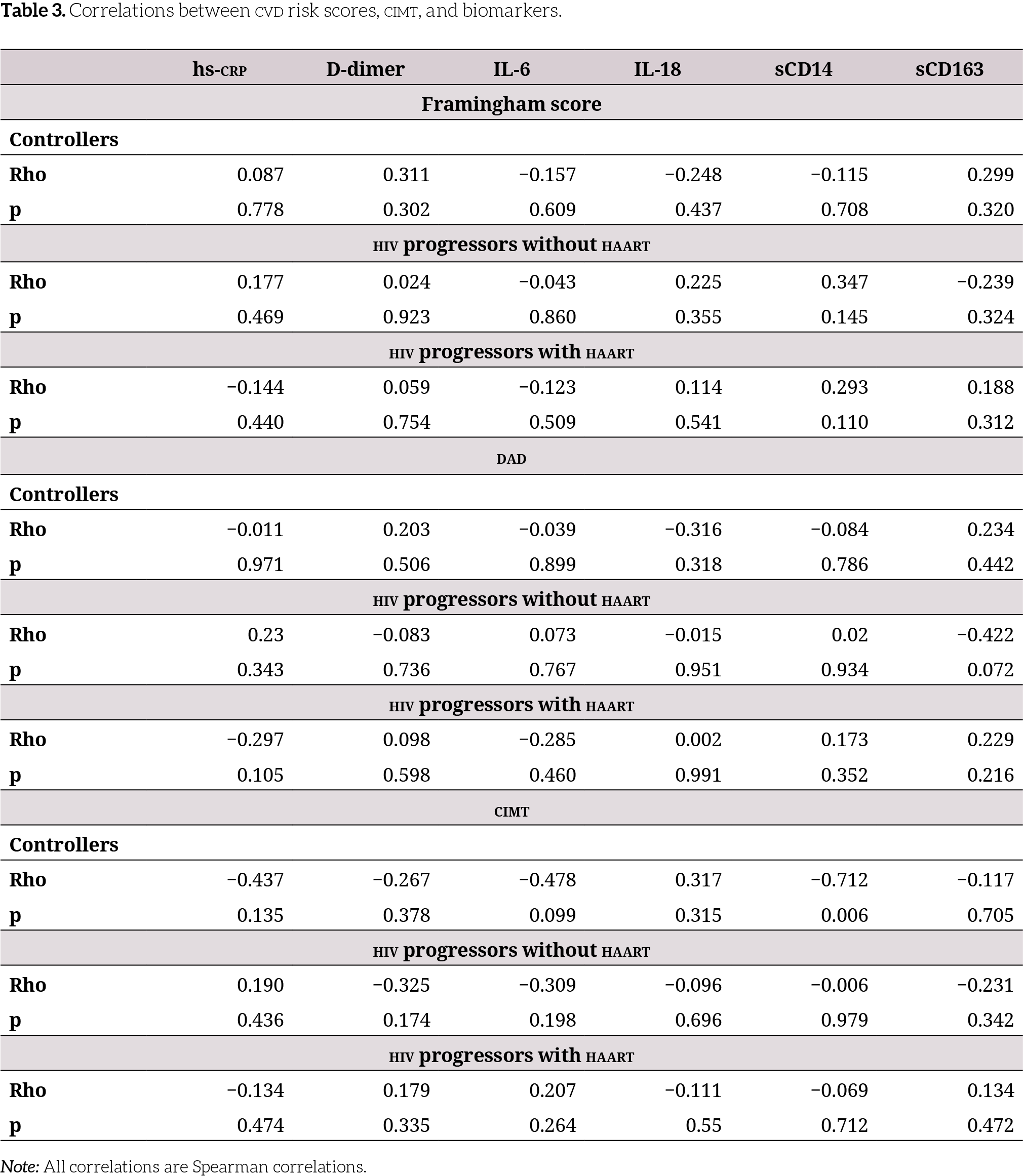
Note: All correlations are Spearman correlations.
Discussion
Cardiovascular disease is emerging as a major cause of morbidity and mortality in patients diagnosed with hiv-1 infection. Recent studies indicate that this risk may be higher by up to 50% (22) in infected individuals, even after adjusting based on traditional risk factors, such as smoking (23). The previously reported high cardiovascular risk in the hiv-1-positive population has been estimated using the Framingham (24) and dad (25) scores. However, this study found no differences among hiv controllers, progressors with and without haart and healthy individuals regarding the estimation of expected cardiovascular risk according to Framingham and dad scores, despite having different progression patterns and viral loads. This could be partly explained by the exclusion of patients with a previous history of cardiovascular disease or diabetes, or by the fact that the recruited population was young. The study has not considered the genetic characteristics of the population either, which could account for changes in the cardiovascular risk scores used. Although previous studies have demonstrated the usefulness of applying Framingham and dad scores to define cvd risk in these patients (26), in this study participants were not categorized as having moderate or high cardiovascular risk. Furthermore, although no differences were found in cimt values in this study, other studies claim that the finding of carotid atherosclerosis would be a better predictor of cvd than various scores (27), so it is possible that prospective studies could contribute in this regard.
On the other hand, previous studies have reported a higher frequency of hypetriglyceridemia and high cholesterol levels in patients with hiv-1 infection compared to the general population (8, 21). This study found that, although below the normal range, hiv progressors with and without haart have higher triglyceride levels when compared with hiv controllers (p < 0.5 and p < 0.01, respectively). In this regard, it has been previously reported that patients with dyslipidemia associated with hiv-1 infection show low levels of hdl and increased total cholesterol, ldl and triglycerides levels, which favor the risk of cardiovascular disease (8). In addition, an association between haart and dyslipidemia has also been suggested, with a greater impact reported in individuals under treatment with protease inhibitors and Stavudine or thymidine analogs in general (28). Specifically, it has been described that haart can increase total cholesterol, ldl cholesterol, and triglyceride levels, having a variable effect on hdl cholesterol levels. In this study population, it was found that hiv progressors without haart have higher triglyceride levels and lower hdl levels compared to the other two groups of patients. Regarding these findings, it is important to highlight that lower hdl levels have been related to increased cardiovascular risk as an independent factor (29). In addition, it was found that in patients receiving haart there are higher hdl levels when compared with individuals not receiving haart or hiv controllers. However, these levels are still significantly lower when compared with the healthy controls. This suggests the possibility that the antiretroviral treatment regimens used by this population have a positive impact on hdl, similar to physical activity or other types of interventions that may influence the levels of this parameter, despite the fact that normal levels are not restored.
haart has been associated with increased prevalence of insulin resistance and risk of diabetes (30). In this study, median fasting glycemia was found to be lower among healthy controls than among patients with hiv-1 infection, suggesting an association with this infection, as noted by other reports.
It has been reported that biomarkers, such as sCD14, sCD163, il-6, high-sensitivity crp, and D-dimer, may play a role in atherogenesis and some of them have been associated with cimt as possible predictors (31). Previous studies mainly comparing patients with hiv-1 infection with non-infected patients have shown that increased sCD14 was associated with increased carotid atheroma plaque formation (rr = 1.24; 95% ci = 1.07- 1.43) (31). Similarly, il-18, which is a proinflammatory, proapoptotic cytokine with atherogenic properties, has been found to be elevated in patients with hiv-1 (32). However, other studies have not reported these differences (33). In this study, no differences were found among the median levels of sCD14, sCD163, il-6, and il18. However, it cannot be ruled out that the low cardiovascular risk of the included population may be one of the reasons for the lack of differences, particularly considering the fact that previous studies have shown that sCD14 levels are lower in infected patients after haart initiation, although they remain high when compared with healthy individuals, and that il-6 may change over time after hiv-1 infection (34).
Other markers, such as high-sensitivity crp, have been used as an important cvd risk prediction tool in the general population, whereas elevated values of D-dimer, a fibrin degradation marker, are reported to be associated with increased mortality in patients with hiv-1 infection (35). In this study, no differences were found among groups of infected patients, but it was observed that patients tended to have higher levels of both biomarkers than healthy controls, although differences were not statistically significant. This may suggest that neither the level of progression nor pharmacological measures can restore these markers to normal values.
On the other hand, in general, no statistically significant correlations were found between Framingham scores, dad values, and other biomarkers. In the hiv controllers group, cimt has a strong negative correlation with the sCD14 marker (Rho = −0.712), which was statistically significant (p = 0.006). This finding contradicts previous publications in which higher levels of sCD14 marker were associated with greater progression of subclinical carotid artery atherosclerosis (31). However, these studies did not differentiate the groups according to the pattern of progression or whether or not they were receiving haart.
It has been reported that some traditional cardiovascular risk scores underestimate cardiovascular risk in patients with hiv-1 infection (36) and the connection of additional markers may improve the performance of these markers. Some of them could be those which are reported in this study, such as hs-crp and D-dimer. Regarding other biomarkers, this result needs to be clarified in other studies, especially in the case of sCD14, which showed negative correlation with cimt in hiv controllers. Finally, follow-up over time of this cohort of patients, whose baseline was established with this study, could provide more information about the cardiovascular behavior of individuals with hiv-1.
hiv-1 infection is an independent factor that increases the risk of cardiovascular events and, despite the initiation of haart, different parameters such as the lipid profile and some biomarkers of inflammation remain altered, which could contribute to the increased risk of cvd. Among these markers, there is evidence of the need to closely monitor triglyceride levels, due to their role as a marker of cvd risk and especially because of the risk of pancreatitis that they represent, as well as to explore the possibility of the emergence of alterations in plasma glycemia and the development of carbohydrate intolerance and diabetes.
Finally, a limitation of the study was the sample size, specifically regarding non-haart hiv progressors and hiv controllers. This is due to the fact that, in our country, consistent with global guidelines, antiretroviral regimens are being started earlier, once the diagnosis of infection is made.
In conclusion, this study found that triglyceride levels were lower in hiv-1 controllers than in hiv progressors, who also present higher viral load and lower cd4+ T lymphocyte counts, especially those without antiretroviral therapy. Although no significant differences were observed in the Framingham, dad, or cimt scores, hiv controllers have a different cardiovascular profile than hiv progressors, according to the metabolic and immunological biomarkers evaluated.
Authors’ contribution
Project formulation: Gustavo Castro, Natalia A. Taborda, Juan C. Hernandez, María Teresa Rugeles, and Fabián Alberto Jaimes. Manuscript preparation: Gustavo Castro, Damariz Marín-Palma, Natalia A. Taborda, Juan C. Hernandez, María Teresa Rugeles, and Fabián Alberto Jaimes. Recruiting of participants: Gustavo Castro, Sarita M. Oyuela, and Kevin León. Clinical evaluation of participants and vascular medicine: Jhon Ubeimar Cataño- Bedoya, Julieta Duque-Botero, and Diana Patricia Giraldo-Méndez. Laboratory tests: Kevin León, Damariz Marín-Palma, Juan C. Hernandez, and María Teresa Rugeles. All authors approved the final version of the manuscript.
The authors would like to thank the following persons for their participation and support.Lorena Andrea Muñoz Guzmán, María Paulina Cortés Palacio, Jhon Erick Ramírez López, Juanita Mesa Abad, and Juan Diego Villa.
Funded by
Immunovirology Group and Department of Internal Medicine, Universidad de Antioquia UdeA; Universidad Cooperativa de Colombia and Corporación Universitaria Remington (4000000116-17).
Conflict of Interest
None declared.
Acknowledgments
The authors would like to thank the following persons for their participation and support: Lorena Andrea Muñoz Guzmán, María Paulina Cortés Palacio, Jhon Erick Ramírez López, Juanita Mesa Abad, and Juan Diego Villa.
References
1. Pelchen-Matthews A, Ryom L, Borges AH, Edwards S, Duvivier C, Stephan C, et al. Aging and the evolution of comorbidities among hiv-positive individuals in a European cohort. Aids. 2018;32(16):2405-16. https://doi.org/10.1097/QAD.0000000000001967
2. Antiretroviral Therapy Cohort C. Causes of death in hiv-1-infected patients treated with antiretroviral therapy, 1996-2006: collaborative analysis of 13 hiv cohort studies. Clin Infect Dis. 2010;50(10):1387-96. https://doi.org/10.1086/652283
3. Ingle SM, May MT, Gill MJ, Mugavero MJ, Lewden C, Abgrall S, et al. Impact of risk factors for specific causes of death in the first and subsequent years of antiretroviral therapy among hiv-infected patients. Clin Infect Dis. 2014;59(2):287-97. https://doi.org/10.1093/ cid/ciu261
4. Sabin CA. Do people with hiv infection have a normal life expectancy in the era of combination antiretroviral therapy? BMC Med. 2013;11:251. https://doi.org/10.1186/1741- 7015-11-251
5. Kuller LH, Tracy R, Belloso W, De Wit S, Drummond F, Lane HC, et al. Inflammatory and coagulation biomarkers and mortality in patients with hiv infection. PLoS Med. 2008;5(10):e203. https://doi.org/10.1371/journal.pmed.0050203
6. Group DADS, Friis-Moller N, Reiss P, Sabin CA, Weber R, Monforte A, et al. Class of antiretroviral drugs and the risk of myocardial infarction. N Engl J Med. 2007;356(17):1723-35. https://doi.org/10.1056/NEJMoa062744
7. Ounjaijean S, Kulprachakarn K, Aurpibul L, Kaewpoowat Q, Boonyapranai K, Chaiwarith R, et al. Cardiovascular risks in Asian hiv-infected patients receiving boosted-protease inhibitor-based antiretroviral treatment. J Infect Dev Ctries. 2021;15(2):289-96. https:// doi.org/10.3855/jidc.12864
8. Estrada V, Martinez-Larrad MT, Gonzalez-Sanchez JL, de Villar NG, Zabena C, Fernandez C, et al. Lipodystrophy and metabolic syndrome in hiv-infected patients treated with antiretroviral therapy. Metabolism. 2006;55(7):940-5. https://doi.org/10.1016/j.metabol.2006.02.024
9. Kirkman MS, Mahmud H, Korytkowski MT. Intensive blood glucose control and vascular outcomes in patients with type 2 diabetes Mellitus. Endocrinol Metab Clin North Am. 2018;47(1):81-96. https://doi.org/10.1016/j.ecl.2017.10.002
10. Beraldo RA, Santos APD, Guimaraes MP, Vassimon HS, Paula FJA, Machado DRL, et al. Body fat redistribution and changes in lipid and glucose metabolism in people living with hiv/aids. Rev Bras Epidemiol. 2017;20(3):526-36. https://doi.org/10.1590/1980- 5497201700030014
11. Lang S, Mary-Krause M, Simon A, Partisani M, Gilquin J, Cotte L, et al. hiv replication and immune status are independent predictors of the risk of myocardial infarction in hiv-infected individuals. Clin Infect Dis. 2012;55(4):600-7. https://doi.org/10.1093/cid/cis489
12. O’Leary DH, Polak JF, Kronmal RA, Manolio TA, Burke GL, Wolfson SK, Jr. Carotid-artery intima and media thickness as a risk factor for myocardial infarction and stroke in older adults. Cardiovascular Health Study Collaborative Research Group. N Engl J Med. 1999;340(1):14-22. https://doi.org/10.1056/NEJM199901073400103
13. Petoumenos K, Reiss P, Ryom L, Rickenbach M, Sabin CA, El-Sadr W, et al. Increased risk of cardiovascular disease (cvd) with age in hiv-positive men: a comparison of the D:A:D cvd risk equation and general population cvd risk equations. hiv Med. 2014;15(10):595- 603. https://doi.org/10.1111/hiv.12162
14. Walker BD. Elite control of hiv infection: implications for vaccines and treatment. Top hiv Med. 2007;15(4):134-6.
15. Feria MG, Taborda NA, Hernandez JC, Rugeles MT. hiv replication is associated to inflammasomes activation, il-1beta, IL-18 and caspase-1 expression in galt and peripheral blood. PloS One. 2018;13(4):e0192845. https://doi.org/10.1371/journal.pone.0192845
16. Taborda NA, Rugeles MT, Montoya CJ. Spontaneous control of hiv replication, but not haart-induced viral suppression, is associated with lower activation of immune cells. J Acquir Immune Defic Syndr. 2014;66(4):365-9. https://doi.org/10.1097/ QAI.0000000000000162
17. Taborda NA, Gonzalez SM, Alvarez CM, Correa LA, Montoya CJ, Rugeles MT. Higher frequency of NK and CD4+ T-Cells in mucosa and potent cytotoxic response in hiv controllers. PloS one. 2015;10(8):e0136292. https://doi.org/10.1371/journal.pone.0136292
18. Friis-Moller N, Thiebaut R, Reiss P, Weber R, Monforte AD, De Wit S, et al. Predicting the risk of cardiovascular disease in hiv-infected patients: the data collection on adverse effects of anti-hiv drugs study. Eur J Cardiovasc Prevent Rehab. 2010;17(5):491-501. https:// doi.org/10.1097/HJR.0b013e328336a150
19. Muñoz OM, Rodríguez NI, Ruiz Á, Rondón M. Validación de los modelos de predicción de Framingham y procam como estimadores del riesgo cardiovascular en una población colombiana. Rev Colomb Cardiol. 2014;21(4):202-12. https://doi.org/10.1016/j. rccar.2014.02.001
20. Muñoz OM, García ÁA, Fernández-Ávila D, Higuera A, Ruiz ÁJ, Aschner P, et al. Guía de práctica clínica para la prevención, detección temprana, diagnóstico, tratamiento y seguimiento de las dislipidemias: evaluación del riesgo cardiovascular. Rev Colomb Cardiol. 2015;22(6):263-9. https://doi.org/10.1016/j.rccar.2015.04.009
21. Marin-Palma D, Castro GA, Cardona-Arias JA, Urcuqui-Inchima S, Hernandez JC. Lower high-density lipoproteins levels during human immunodeficiency virus type 1 infection are associated with increased inflammatory markers and disease progression. Front Immunol. 2018;9:1350. https://doi.org/10.3389/fimmu.2018.01350
22. Feinstein MJ, Bahiru E, Achenbach C, Longenecker CT, Hsue P, So-Armah K, et al. Patterns of cardiovascular mortality for hiv-infected adults in the United States: 1999 to 2013. Am J Cardiol. 2016;117(2):214-20. https://doi.org/10.1016/j.amjcard.2015.10.030
23. Mdodo R, Frazier EL, Dube SR, Mattson CL, Sutton MY, Brooks JT, et al. Cigarette smoking prevalence among adults with hiv compared with the general adult population in the United States: cross-sectional surveys. Ann Intern Med. 2015;162(5):335-44. https://doi. org/10.7326/M14-0954
24. Durand M, Chartrand-Lefebvre C, Baril JG, Trottier S, Trottier B, Harris M, et al. The Canadian hiv and aging cohort study - determinants of increased risk of cardio-vascular diseases in hiv-infected individuals: rationale and study protocol. BMC Infect Dis. 2017;17(1):611. https://doi.org/10.1186/s12879-017-2692-2
25. Law M, Friis-Moller N, Weber R, Reiss P, Thiebaut R, Kirk O, et al. Modelling the 3-year risk of myocardial infarction among participants in the Data Collection on Adverse Events of Anti-hiv Drugs (dad) study. hiv Med. 2003;4(1):1-10. https://doi.org/10.1046/j.1468- 1293.2003.00138.x
26. Thompson-Paul AM, Lichtenstein KA, Armon C, Palella FJ, Jr., Skarbinski J, Chmiel JS, et al. Cardiovascular Disease Risk Prediction in the hiv Outpatient Study. Clin Infect Dis. 2016;63(11):1508-16. https://doi.org/10.1093/cid/ciw615
27. Phan BAP, Weigel B, Ma Y, Scherzer R, Li D, Hur S, et al. Utility of 2013 American College of Cardiology/American Heart Association Cholesterol Guidelines in hiv-infected adults with carotid atherosclerosis. Circ Cardiovasc Imaging. 2017;10(7). https://doi.org/10.1161/ CIRCIMAGING.116.005995
28. Nsagha DS, Weledji EP, Assob NJ, Njunda LA, Tanue EA, Kibu OD, et al. Highly active antiretroviral therapy and dyslipidemia in people living with hiv/aids in Fako Division, South West Region of Cameroon. BMC Cardiovasc Dis. 2015;15:95. https://doi.org/10.1186/ s12872-015-0090-5
29. Hassan M, Philip P. canheart: is HDL cholesterol a cardiovascular specific risk factor? Glob Cardiol Sci Pract. 2016;2016(4):e201634. https://doi.org/10.21542/gcsp.2016.34
30. Araujo S, Banon S, Machuca I, Moreno A, Perez-Elias MJ, Casado JL. Prevalence of insulin resistance and risk of diabetes mellitus in hiv-infected patients receiving current antiretroviral drugs. Eur J Endocrinol. 2014;171(5):545-54. https://doi.org/10.1530/EJE-14-0337
31. Hanna DB, Lin J, Post WS, Hodis HN, Xue X, Anastos K, et al. Association of macrophage inflammation biomarkers with progression of subclinical carotid artery atherosclerosis in hiv-infected women and men. J Infect Dis. 2017;215(9):1352-61. https://doi.org/10.1093/ infdis/jix082
32. Iannello A, Boulassel MR, Samarani S, Tremblay C, Toma E, Routy JP, et al. hiv-1 causes an imbalance in the production of interleukin-18 and its natural antagonist in hiv-infected individuals: implications for enhanced viral replication. J Infect Dis. 2010;201(4):608-17. https://doi.org/10.1086/650314
33. Marin-Palma MD, Cardona-Arias MJA, Hernández SDJC. Factores inmunológicos relacionados con vih-1 en pacientes colombianos. Rev Cienc Salud. 2019;17(2). https://doi. org/10.12804/revistas.urosario.edu.co/revsalud/a.7927
34. Sereti I, Krebs SJ, Phanuphak N, Fletcher JL, Slike B, Pinyakorn S, et al. Persistent, albeit reduced, chronic inflammation in persons starting antiretroviral therapy in acute hiv infection. Clin Infect Dis. 2017;64(2):124-31. https://doi.org/10.1093/cid/ciw683
35. Rugeles-López MT, Oyuela-Gómez SM, Castro-Torres GA, Jaimes-Barragán FA. Biomarcadores inmunológicos de riesgo cardiovascular en la infección por el virus de inmunodeficiencia humana-1. Rev Colomb Cardiol. 2017;24(2):153-60. https://doi. org/10.1016/j.rccar.2016.05.012
36. Hanna DB, Post WS, Deal JA, Hodis HN, Jacobson LP, Mack WJ, et al. hiv infection is associated with progression of subclinical carotid atherosclerosis. Clin Infect Dis. 2015;61(4):640-50. https://doi.org/10.1093/cid/civ325
Author notes
* Corresponding author: fabian.jaimes@udea.edu.co