

Effectiveness of Chlorhexidine and Essential Oils Associated with Scaling and Root Planing in the Treatment of Chronic Periodontitis
Efectividad de la clorhexidina y aceites esenciales asociados al raspado y alisado radicular en el tratamiento de periodontitis crónica
Efetividade da clorexidina e aceites essenciais associados à raspagem e alisamento radicular no tratamento de periodontite crónica
Effectiveness of Chlorhexidine and Essential Oils Associated with Scaling and Root Planing in the Treatment of Chronic Periodontitis
Revista Ciencias de la Salud, vol. 18, no. 3, 2020
Universidad del Rosario
Received: 21 january 2020
Accepted: 24 july 2020
Additional information
To cite this article: León Rodríguez JA, Vargas Casana ST, Millones Gómez PA. Effectiveness of Chlorhexidine and Essential Oils Associated with Scaling and Root Planing in the Treatment of Chronic Periodontitis. Rev Cienc Salud. 2020;18(3):1-11. https://doi.org/10.12804/revistas.urosario.edu.co/revsalud/a.9795
Abstract: Introduction: Adjunctive treatment for periodontal disease is quite varied and depends on many factors. This study aims to compare the effectiveness of 0.12% chlorhexidine and essential oils associated with scaling and root planing in the treatment of chronic periodontitis. Material and methods: The sample included 42 patients randomly assigned to three groups. Decrease in periodontal status was measured with the World Health Organization’s periodontal probe by analyzing probe depth values and level of clinical insertion at 3, 4, and 5 months. Statistical analysis of the progress of the three therapies was conducted using Student’s ., Anova, and Tukey tests with a significance level of . < 0.05. Results: The obtained values demonstrated that 0.12% chlorhexidine is more effective in all of its follow ups, whereas no significant difference existed between essential oils and the control group. A significant difference was observed over time in each separate treatment. Conclusion: Chlorhexidine at a 0.12% concentration associated with root scaling and planing is better than essential oil therapies for the treatment of chronic periodontitis.
Keywords: Chlorhexidine, essential oils, mouthwash, chronic periodontitis.
Resumen: Introducción: el tratamiento coadyuvante de la enfermedad periodontal es muy variado y depende de muchos factores. El objetivo del presente artículo fue comparar la efectividad entre clorhexidina al 0.12 % y aceites esenciales asociados al raspado y alisado radicular en el tratamiento de periodontitis crónica. Materiales y métodos: la muestra estuvo conformada por 42 pacientes distribuidos aleatoriamente en 3 grupos. La disminución del estado periodontal se midió con la sonda periodontal de la Organización Mundial de la Salud, analizando los valores profundidad al sondaje y el nivel de inserción clínica a los 3, 4 y 5 meses. Para el análisis estadístico de la evolución de las 3 terapias se empleó la . de Student, análisis de varianza y test de Tukey con un nivel de significancia de . < 0.05. Resultados: los valores obtenidos demostraron que la clorhexidina al 0.12 % es más efectiva en todos sus controles; mientras que no existe diferencia significativa entre aceites esenciales y el grupo control. Existe diferencia significativa a través del tiempo en cada tratamiento por separado. Conclusión: la clorhexidina al 0.12 % asociada al raspado y alisado radicular es superior a los tratamientos con aceites esenciales en el tratamiento de la periodontitis crónica.
Palabras clave: clorhexidina, aceites esenciales, enjuague bucal, periodontitis crónica.
Resumo: Introdução: o tratamento coadjuvante da doença periodontal . muito variado e depende de muitos fatores. O objetivo do presente estudo foi comprar a efetividade entre clorexidina ao 0.12% e aceites essenciais associados à raspagem e alisamento radicular no tratamento de periodontite crónica. Materiais e métodos: a amostra esteve conformada por 42 pacientes distribuídos aleatoriamente em 3 grupos. A diminuição de estado periodontal se mediu com a sonda periodontal as Organização Mundial da Saúde analisando os valores profundidade à sondagem e nível de inserção clínica aos 3, 4 e 5 meses. A análise estatística da evolução das 3 terapias, se realizou empregando . de Student, Anova e teste de Tukey com um nível de significância de . < 0.05. Resultados: os valores obtidos demostraram que a clorexidina ao 0.12% é mais efetiva em todos seus controles, enquanto não existe diferença significativa entre aceites essenciais e o grupo controle. Existe diferença significativa através do tempo em cada tratamento por separado. Conclusão: a clorexidina ao 0.12% associada à raspagem e alisamento radicular é superior aos tratamentos com aceites essenciais no tratamento da periodontite crónica.
Palavras-chave: clorexidina, aceites essenciais, enxaguante bucal, periodontite crónica.
Introduction
Periodontitis is an infectious pathology whose main characteristic is the formation of periodontal pockets or gingival recession, which is caused by inflammation and destruction of the supporting and surrounding dental structure (1-3). Severe periodontitis causes tooth loss and is very common; it is prevalent in 10% of the population worldwide (4).
Literature consistently states the importance of supragingival plaque control due to its positive effect on periodontal disease, which has been demonstrated for a long time. Mechanical plaque control is the most common form of oral hygiene; however, individual mechanical control has limitations, especially in terms of skill and motivation (5, 6).
Several substances such as natural products, systemic antibiotics, and chemical solutions have been used to compensate these limitations, with interesting results being obtained. Mouthwash used therapeutically is a complement to regular hygiene, brushing, and daily flossing (7, 8).
Control of the supragingival plate considerably increases when mouthwashes are used as adjuvants to scaling and root planing, and they have a positive effect on subgingival bacterial recolonization. Chlorhexidine is the gold standard for periodontal disease control, since it inhibits plaque formation and is effective in preventing and controlling biofilm formation (9,10).
Essential oils have also been shown to have antibacterial activity and antiplaque effect. They have been used in candies and mouthwashes for years, the best known being Listerine®, which is an essential oil product composed of a mixture of thymol, menthol and eucalyptol combined with methyl salicylate and 26.9% alcohol and is available in different flavors (11-14).
Miley et al. conducted a prospective, randomized, double-blind trial to evaluate the efficacy of Smart Mouth Clinical dds mouthwash compared to 0.12% chlorhexidine and placebo mouthwash; their sample comprised 66 individuals randomized to receive any of the study rinses (15). The measuring instruments used were gingival index, bleeding index, and plaque index. Assessments were performed at 3 and 6 weeks. The results showed a significant decrease at 3 and 6 weeks in all groups. Differences between groups were not statistically significant. Clinical improvement was observed in all study groups.
Haerian et al. compared the antimicrobial effectiveness of three different mouthwashes. Supragingival plaque samples were collected from 32 patients, which were placed on agar plates and discs previously immersed in the three mouthwashes (16). The zone of bacterial inhibition (ZOI) was measured after incubation for 24 h. Moreover, in vivo effectiveness was compared, and patients rinsed with 0.2% Chlorhexidine and Listerine® (for monotherapies); the control group rinsed with water. The procedure was performed for 2 weeks and new plaque samples were collected to count colony forming units (CFU). Haerian et al. concluded that 0.2% chlorhexidine considerably reduces bacterial growth and that the three rinses produce changes after 2 weeks, although with different degrees of effectiveness (16).
Garcia et al. conducted a prospective, randomized, double-blind trial comparing the effectiveness of two mouthwashes based on chlorhexidine and cetylpyridinium chloride after scaling and root planing (17). Their sample was comprised of 30 individuals and was divided into 3 groups. The first group was administered 0.12% chlorhexidine and 0.05% cetylpyridinium chloride, the second group received 0.03% chlorhexidine and 0.05% cetylpyridinium chloride, and the third one was the positive control group. All individuals were instructed to rinse after scaling and root planing and improvement was assessed at the first month. They concluded that rinsing with 0.12% chlorhexidine and 0.05% cetylpyridinium chloride shows a higher effect in lowering the level of plaque as opposed to the other monotherapies.
Alshehri et al. conducted a systematic review to determine the effectiveness of essential oils (Listerine) for improving periodontal status. Out of the 26 studies, only 13 support the long-term effectiveness of Listerine during a 3–6 months period as a complement to scaling and root planing. They concluded that essential oils provide an excellent anti-plaque effect and reduce gingival inflammation as a complement to mechanical plaque control (14).
Vlachojannis et al. conducted a systematic review on the therapeutic benefits and safety of Listerine®. In the review, they included the evaluation of the effect of mouthwash for 6 months and concluded that it is effective for the improvement of periodontal health (12).
The key to successful periodontal treatment is the absence of both inflammation and destruction of the supporting tissues of the tooth. Often, scaling and root planing is not sufficient for controlling the disease, but adjuvant therapies are an excellent complement to mechanical plaque control. This study aims to evaluate two mouthwashes associated with scaling and root planing and to compare their effectiveness in patients with chronic periodontitis.
Materials and Methods
This is an experimental, prospective, longitudinal, and analytical triple-blind study. The study participants included patients of the Periodontics Department of the uladech Dental Care Teaching Clinic, in Trujillo, from August to December 2015. The sample comprised 42 patients divided into three groups (18).
Inclusion criteria were patients between 30 and 50 years old, with no systemic disease, periodontal pockets of ≥5 mm deep, and a minimum of 15 teeth.
Patients with prior periodontal treatment 5 months before initiation were excluded from the study; smokers, alcoholics, and drug addicts of any condition as well as pregnant and nursing women were also excluded.
This study was approved by the Dental School Ethics Committee of Universidad Católica los Angeles de Chimbote, considering the principles of the Declaration of Helsinki and the General Health Act of Peru (Act No. 268429) (19).
Since this was a triple-blind study, an operator labeled the containers with mouthwash as mouthwash A and mouthwash B. To avoid the possibility of bias, this operator was responsible for disclosing the results at the end of the study. The type of mouthwash prescribed was not revealed to the patients, statistician, and clinician.
The Hu-Friedy® who periodontal probe was used. Furthermore, to homogenize the sample, all patients were instructed in the bass brushing technique. oral b brand brushes and 90-g triclosan-free Kolynos Herbal toothpaste were provided. All patients were summoned every 45 days to reinforce brushing instructions and to replenish their toothpaste. The sample was divided into three groups with 14 individuals each.
Group A: Scaling and root planing were performed and mouthwash A (0.12% chlorhexidine, 0.12% perioaid) was prescribed for 2 weeks.
Group B: Scaling and root planing was performed and mouthwash B (essential oils, Listerine®) was prescribed for 2 weeks.
Group C: Only scaling and root planing was performed, and it was considered the control group.
Indications for both mouthwashes were to rinse with 10 ml for 1 min, twice a day, in the morning and at night after brushing, for 2 weeks.
Scaling and root planing was performed with Hu-Friedy® brand Grayce curettes: 1-2, 3-4, and 5-6 for anterior teeth and free surfaces, and 11-12 and 13-14 for distal and mesial posterior teeth.
Teeth that met the inclusion criteria for depth upon probing (5 mm or more) were assessed as in study initiation to observe clinical improvements. Probe depth was assessed by evaluating the distance in millimeters from the gingival margin to the base of the periodontal pocket and gain in clinical insertion level was assessed by evaluating the distance in millimeters from the enamel cement junction to the base of the periodontal pocket. Assessments were long-term and were conducted at 3, 4, and 5 months.
The effectiveness of 0.12% chlorhexidine, essential oil, and the control group was compared using Anova and Tukey’s test for multiple comparisons between treatments with a level of significance of .< 0.05.
Results
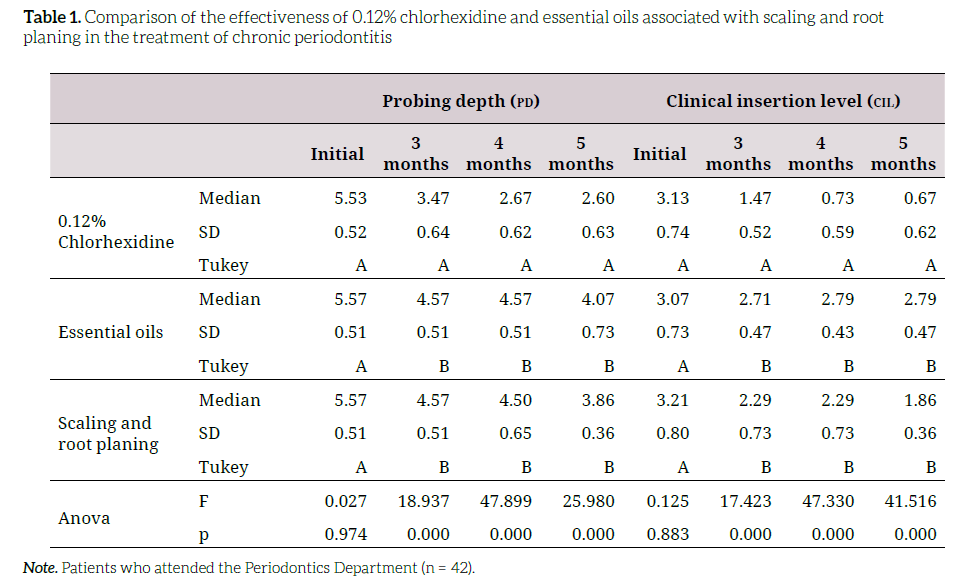
The values of periodontal status decrease, including probing depth (PD) and gain in clinical insertion level (CIL), are shown for the three analyzed therapies: 0.12% chlorhexidine, essential oils, and scraping and root planing alone. The three therapies had a statistically significant difference (p = 0.000) at 3, 4, and 5 months. Moreover, the probing depth values at 3, 4, and 5 months were lower with 0.12% chlorhexidine than with essential oils and the control group. Tukey’s test indicated that there was no difference between groups in terms of both initial probing depth measurements and clinical insertion level gain (A). However, the essential oils group and the scraping and root planing group did not show differences at 3, 4, and 5 months (B) but showed a significant difference from all the chlorhexidine groups at 3, 4, and 5 months (Table 1).
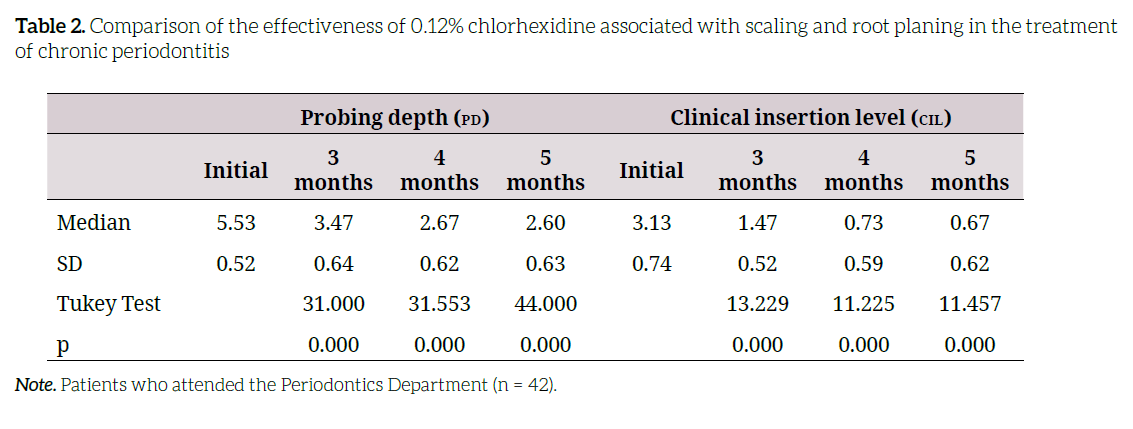
The effectiveness of 0.12% chlorhexidine regarding initial status is associated with a decrease in probing depth and a gain in the level of clinical insertion at 3, 4, and 5 months (p < 0.05, in each case) (Table 2).
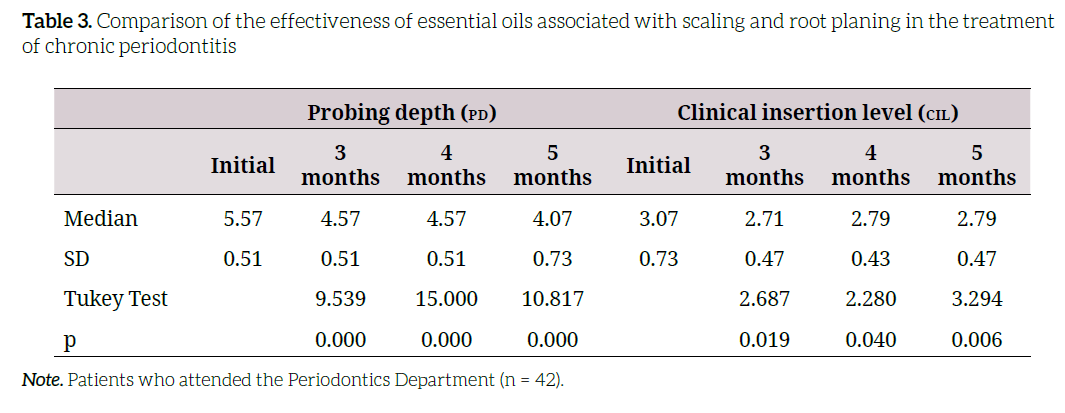
The effectiveness of essential oils regarding initial status is associated with a decrease in probing depth and a gain in the level of clinical insertion at 3, 4, and 5 months (p < 0.05, in each case) (Table 3).
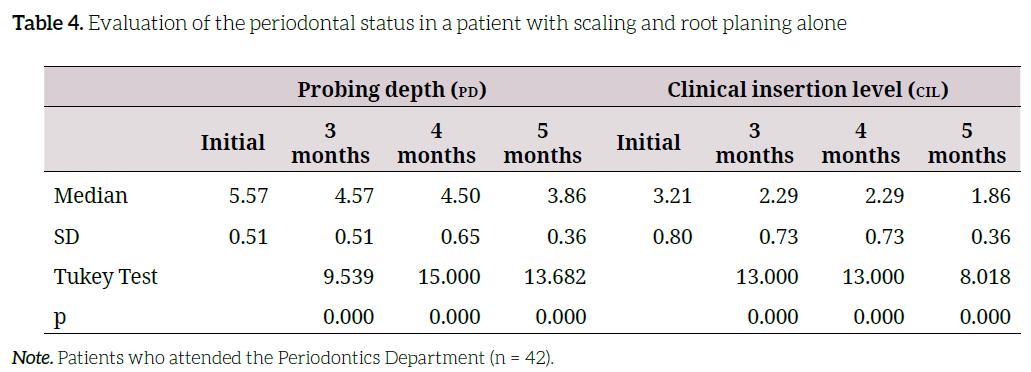
The initial status for scaling and root planing therapy alone is associated with a decrease in probing depth and a gain in the level of clinical insertion at 3, 4, and 5 months (p < 0.05, in each case) (Table 4).
Discussion
Scaling and root planing is a procedure by which plaque and calculi are removed from supragingival and subgingival tooth surfaces; root planing, consequently, removes calculi and adhered portions of residual cementum from the roots to create a smooth and clean surface. This treatment restores periodontal health and completely removes the elements that produce gingival inflammation; it also eliminates microorganisms and leads to a change in subgingival plaque composition (20).
In this study, 0.12% chlorhexidine and essential oils were chosen because of their adjunctive effect on scaling and root planing in periodontal treatment and because they are widely used in dentistry as monotherapies together with mechanical therapy for periodontal treatment (21-23).
Periodontal destruction due to inflammation causes rupture of the connective tissue. The greatest destruction in this process, however, is mediated by the host’s immune system. Moreover, 0.12% chlorhexidine has a bactericidal effect and is the gold standard in periodontal treatment (24).
For some time, periodontal treatment has been conducted only by mechanical methods. However, since periodontal diseases appear to be specific infections caused by a proliferation of a particular microbiological component and not of all the subgingival plaque species, it seems logical that the flora can be eliminated in a biological and specific way with an antimicrobial agent in association with a mechanical debridement of root surfaces (25-29).
This study demonstrated that the use of 0.12% chlorhexidine in association with scraping and root planing achieved a significantly higher effectiveness compared to essential oils and mechanical treatment of plaque alone (monotherapies) at 3, 4, and 5 months, thus constituting an excellent therapeutic option.
Mouthwashes are often prescribed by dentists; however, a range of mouthwashes are available over the counter and are used by patients without professional supervision. Like all pharmacological substances, patients should consider not only their positive effects but also their most relevant side effects and possible negative consequences (25-29).
The effectiveness of chlorhexidine in preventing initial plaque formation and dispersion of preformed plaque has made it the drug of choice for large clinical situations where conventional daily oral hygiene techniques are difficult to perform. Therefore, they have been used in cases where there is difficulty in performing proper hygiene as well as in orthodontic treatments where adequate brushing is difficult and can easily lead to gingivitis and periodontal involvement. Therefore, chlorhexidine can be used as an alternative method for plaque control (30).
We concluded that 0.12% chlorhexidine in association with scaling and root planing was more effective than essential oil monotherapies and mechanical plaque control alone at 3, 4, and 5 months after scaling and root planing.
Referencias
1. Natto Z, Ahmad R, Alsharif L, Alrowithi H, Alsini D, Salih H, et al. Chronic periodontitis case definitions and confounders in periodontal research: A systematic assessment. Biomed Res Int. 2018;2018:1-9. https://doi.org/10.1155/2018/4578782
2. Van der Weijden G, Dekkers G, Slot D. Éxito de la terapia periodontal no quirúrgica en pacientes adultos con periodontitis: un análisis retrospectivo. Int J Dent Hyg. 2019;17(4):309317. https://doi.org/10.1111/idh.12399
3. Preshaw P. Detección y diagnóstico de afecciones periodontales susceptibles de prevención. bmc Salud Oral. 2015;15(1):1-11 https://doi.org/10.1186/1472-6831-15-S1-S5
4. Organización Mundial de la Salud. Salud bucodental [internet]. Ginebra: Organización; 2020. Available from: https://www.who.int/es/news-room/fact-sheets/detail/oral-health
5. Rösing C, Cavagni J, Gaio E, Muniz F, Ranzan N, Oballe H, et al. Eficacia de dos colutorios con cloruro de cetilpiridinio: un ensayo clínico aleatorizado controlado. Braz Res Oral. 2017;31:e47. https://doi.org/10.1590/1807-3107bor-2017.vol31.0047
6. Takenaka S, Ohsumi T, Noiri Y. Evidence-based strategy for dental biofilms: Current evidence of mouthwashes on dental biofilm and gingivitis. Jpn Dent Sci Rev. 2019;55(1):3340. https://doi.org/10.1016/j.jdsr.2018.07.001
7. Colussi PR, Haas AN, Oppermann RV, Rösing CK. Consumo de pasta dental y factores asociados en un grupo de población brasileño. Cad Saude Publica. 2011;27(3):546-54. https://doi.org/10.1590/S0102-311X2011000300014
8. Lynch MC, Cortelli SC, McGuire JA, Zhang J, Ricci-Nittel D, Mordas CJ, et al. The effects of essential oil mouthrinses with or without alcohol on plaque and gingivitis: A randomized controlled clinical study. bmc Oral Health. 2018;18(1):6. https://doi.org/10.1186/s12903-017-0454-6
9. Fernandez M, Exterkate R, Bujis M, Crielaard, Zaura E. Effect of mouthwashes on the composition and metabolic activity of oral biofilms grown in vitro. Clin Oral Investig. 2017;21(4):1221-30. https://doi.org/10.1007/s00784-016-1876-2
10. Sakaue Y, Takenaka S, Ohsumi T, Domon H, Terao Y, Noiri Y. The effect of chlorhexidine on dental calculus formation: An in vitro study. bmc Oral Health. 2018;18(1):1-7. https:// doi.org/10.1186/s12903-018-0517-3
11. Quintas V, Prada I, Donos N, Suárez D, Tomás I. Antiplaque effect of essential oils and 0.2% chlorhexidine on an in situ model of oral biofilm growth: A randomised clinical trial. PLoS One. 2015;10(2):1-18. https://doi.org/10.1371/journal.pone.0117177
12. Vlachojannis C, Al-Ahmad A, Hellwig E, Chrubasik S. Listerine products: An update on the efficacy and safety. Phytother Res. 2016;30(3):367-73. https://doi.org/10.1002/ptr.5555
13. Marchetti E, Tecco S, Caterini E, Casalena F, Quinzi V, Mattei A, et al. Alcohol-free essential oils containing mouthrinse efficacy on three-day supragingival plaque regrowth: A randomized crossover clinical trial. Trials. 2017;18(1):1-8. https://doi.org/10.1186/s13063-017-1901-z
14. Alshehri FA. The use of mouthwash containing essential oils (listerine) to improve oral health: A systematic review. Arabia Dent J. 2018 enero;30(1):2-6. https://doi.org/10.1016/j. sdentj.2017.12.004
15. Miley DD, Garcia MN, Omran MT, Binz ED, Fortino DJ, Siterlet AC, Hildebolt CF. Comparative evaluation of smartmouth clinical dds advanced oral rinse and chlorhexidine mouthrinse. Oral Health Prev Dent. 2019;17(4):339-47. https://doi.org/10.3290/j.ohpd.a42504
16. Haerian A, Rezaei M, Talebi M, Keshavarz N, Amid R, Meimandi M. Comparison of antimicrobial effects of three different mouthwashes. Iran J Public Health. 2015;44(7):997-1003.
17. García M, Zurlohe M, Montero E, Alonso B, Serrano J, Sanz M, et al. Evaluation of new chlorhexidine-and cetylpyridinium chloride-based mouthrinse formulations adjunctive to scaling and root planing: pilot study. Int J Dent Hyg. 2017;15(4):269-279. https://doi.org/10.1111/idh.12254
18. Dawson B, Trapp G. Bioestadística médica. 4.ª ed. Ciudad de México: Manual Moderno; 2005.
19. Declaración de Helsinki de la amm. Principios éticos para las investigaciones médicas en seres humanos. Asociación Médica Mundial [internet]. 2013 [citado 2019 Nov 22]. Available from: https://www.isciii.es/QueHacemos/Servicios/ComitesEtica/CEI/Documents/Declaracion-Helsinki-2013-Esp.pdf#search=helsinki
20. Pensantes-Sangay S, Calla-Poma R, Requena-Mendizábal M, Alvino-Vales M, MillonesGómez P. Chemical composition and antibacterial effect of plantago major extract on periodontal pathogens. Pesqui Bras Odontopediatria Clín Integr. 2020;20:e0012. https:// doi.org/10.1590/pboci.2020.100
21. Jafer M, Patil S, Hosmani J, Bhandi SH, Chalisserry EP, Anil S. Chemical plaque control strategies in the prevention of biofilm-associated oral diseases. J Contemp Dent Pract. 2016;17(4):337-43. https://doi.org/10.5005/jp-journals-10024-1851
22. Cosyn J, Princen K, Miremadi R, Decat E, Vaneechoutte M, De Bruyn H. Antimicrobial effect of newly formulated toothpastes and a mouthrinse on specific microorganisms: An in vitro study. Eur J Dent. 2019;13(2):172-77. https://doi.org/10.1055/s-0039-1695655
23. Tartaglia GM, Tadakamadla SK, Connelly ST, Sforza C, Martín C. Adverse events associated with home use of mouthrinses: A systematic review. Ther Adv Drug Saf. 2019;10(1):1-16. https://doi.org/10.1177/2042098619854881
24. Prietto NR, Martins TM, Santinoni CD, Pola NM, Ervolino E, Bielemann AM, Leite FR. Treatment of experimental periodontitis with chlorhexidine as adjuvant to scaling and root planing. Arch Oral Biol. 2019;1(1):1-24. https://doi.org/10.1016/j.archoralbio.2019.104600
25. Becerra TB, Calla-poma RD, Requena-Mendizábal MF. Antibacterial effect of Peruvian propolis collected during different seasons on the growth of streptococcus mutans. Open Denti J. 2019;13:2019:327-31. https://doi.org/10.2174/1874210601913010327
26. Bacilio-Amaranto R, Millones P. Analgesic effectiveness of lysine clonixinate associated with paracetamol in the postoperative treatment of exodontias. Rev Cienc Salud. 2019;17(2):321-33. https://doi.org/10.12804/revistas.urosario.edu.co/revsalud/a.7943
27. Balejo RD, Cortelli JR, Costa FO, Cyrino RM, Aquino DR, Cogo K, Miranda TB, Moura SP, Cortelli SC. Effects of chlorhexidine preprocedural rinse on bacteremia in periodontal patients: a randomized clinical trial. J Appl Oral Sci. 2017;25(6):586-595. https://doi.org/10.1590/1678-7757-2017-0112
28. Da Costa LF, Amaral CD, Barbirato DD, Leão AT, Fogacci MF. Chlorhexidine mouthwash as an adjunct to mechanical therapy in chronic periodontitis: A meta-analysis. J Am Dent Assoc. 2017;148(5):308-18. https://doi.org/10.1016/j.adaj.2017.01.021
29. Millones-Gómez P, Huamaní-Muñoz W. Efectividad de la antibioticoterapia en la reducción de la frecuencia de alveolitis seca postexodoncia simple: ensayo clínico aleatorizado de grupos en paralelo, controlado y ciego simple. Rev Esp Cirug Oral Maxilofac. 2016;38(4):181-7. https://doi.org/10.1016/j.maxilo.2014.04.004
30. Millones P, Aguirre A. Efficacy of azithromycin associated with rar in chronic periodontitis: Clinical trial, randomized, controlled, triple blind parallel groups. Rev Esp Cirug Oral Maxilofac. 2018;40(3):129-34. http://dx.doi.org/10.1016/j.maxilo.2017.08.001
Notes
Conflict of Interest None declared.
Contribution of authors Jhair Alexander León Rodríguez and Sandra Thays Vargas Casana: participated in the conception and design of this paper, in the data analysis and interpretation processes, in the drafting and critical review of this paper and in the approval of its final version. Pablo Alejandro Millones Gómez: participated in the data analysis and interpretation processes, in the conception and design of this paper, and in the approval of its final version.
Author notes
a Corresponding author: pablodent@hotmail.com