

Perceptions of Individuals with Parkinson’s Disease about Quality of Life
Percepciones de pacientes con enfermedad de Parkinson sobre la calidad de vida
Percepções de pacientes com doença de Parkinson sobre a qualidade de vida
Perceptions of Individuals with Parkinson’s Disease about Quality of Life
Revista Ciencias de la Salud, vol. 16, no. 2, 2018
Universidad del Rosario
Received: 16 May 2017
Accepted: 26 February 2018
Additional information
To cite this
article: Foppa AA, Vargas-Peláez CM, Buendgens BF, Chemello C, Charmillot FMP, Marin
M, et al. Perceptions of Individuals with Parkinson’s Disease about Quality of
Life. Rev Cienc
Salud. 2018;16(2):262-278. Doi: https://doi.org/10.12804/revistas.urosario.edu.co/revsalud/a.6769
Abstract: Introduction: Parkinson’s disease is a neurodegenerative disorder manifested by motor and non-motor symptoms that compromise patients’ quality of life. The instrument used to assess Parkinson’s disease patients’ quality of life is the Parkinson’s Disease Questionnaire (PDQ-39). This study aims to identify issues related to quality of life from the patients’ perspective, compare the results obtained with the aspects included in the PDQ-39, and describe some strategies that patients have adopted to overcome difficulties. Materials and methods: This is a qualitative and descriptive study based on a focus group consisting of six patients. Data were analyzed using the content analysis method. Results: Aspects related to all PDQ-39 domains were mentioned by the patients, highlighting those related to limitations on their mobility and daily activities, as well as aspects related to their emotional wellbeing. The patients did not mention some aspects of mobility that are included in the PDQ-39, but limitations in the domain of emotional wellbeing that are included in the PDQ-39 were detected. In order to overcome difficulties, patients devise various strategies that require social support. Conclusion: Understanding and reflecting on Parkinson’s disease patients’ perceptions of their quality of life contributes to our understanding of the disease and stimulates proposals for adequate clinical interventions to provide comprehensive care. It is suggested that the PDQ-39 be reviewed and adapted to the current context, taking into account the most recent knowledge and technological advances related to Parkinson’s disease.
Keywords: quality of life, Parkinson disease, PDQ-39.
Resumen: Introducción: la enfermedad de Parkinson es una patología neurodegenerativa, que se manifiesta por signos y síntomas motores y no motores, que comprometen la calidad de vida de los pacientes. El Parkinson Disease Questionnaire (PDQ-39) es el instrumento más utilizado para evaluar la calidad de vida en pacientes con esta enfermedad. Los objetivos del trabajo fueron identificar los aspectos relacionados con la Calidad de Vida desde la perspectiva de los pacientes, compararlos con los aspectos considerados por el PDQ-39 y describir las estrategias adoptadas por los pacientes para superar las dificultades. Materiales y métodos: estudio cualitativo, descriptivo. Se realizó un grupo focal con seis pacientes. Los datos fueron analizados usando el método de análisis de contenido. Resultados: aspectos relacionados a todos los dominios del PDQ-39 fueron mencionados por los pacientes, destacándose aquellos relacionados con las limitaciones de la movilidad y el desarrollo de actividades diarias, y aspectos relacionados con el bienestar emocional. No obstante, algunos aspectos considerados en el dominio movilidad del PDQ-39 no fueron mencionados, y fueron detectadas limitaciones del dominio bienestar emocional. Los pacientes diseñan diversas estrategias para superar las dificultades, en las que el soporte social es importante. Conclusión: conocer y reflexionar sobre las percepciones de persona con enfermedad de Parkinson sobre su calidad de vida contribuye para la comprensión de la enfermedad y auxilia la propuesta de intervenciones clínicas adecuadas para lograr el cuidado integral. Se sugiere la revisión y adaptación del PDQ-39 al contexto actual, los avances tecnológicos y de conocimientos sobre la enfermedad de Parkinson.
Palabras clave: calidad de vida, enfermedad de Parkinson, PDQ-39.
Resumo: Introdução: a doença de Parkinson é uma patologia neurodegenerativa, que se manifesta por signos e sintomas motores e não motores, que comprometem a qualidade de vida dos pacientes. O Parkinson Disease Questionnaire (PDQ-39) é o instrumento mais utilizado para avaliar a qualidade de vida de em pacientes com esta doença. Os objetivos do trabalho foram identificar os aspetos relacionados com a Qualidade de Vida desde a perspectiva dos pacientes, compará-los com os aspetos considerados pelo PDQ-39 e descrever as estratégias adotadas pelos pacientes para superar as dificuldades. Materiais e métodos: estudo qualitativo, descritivo. Realizou-se um grupo focal com seis pacientes. Os dados foram analisados usando o método de análise de conteúdo. Resultados: aspetos relacionados a todos os domínios do PDQ-39 foram mencionados pelos pacientes, destacando-se aqueles relacionados com as limitações da mobilidade e o desenvolvimento de atividades diárias, e aspetos relacionados com o bem-estar emocional. No entanto, alguns aspectos considerados no domínio mobilidade do PDQ-39 não foram mencionados, e foram detectadas limitações do domínio bem-estar emocional. Os pacientes desenham diversas estratégias para superar as dificuldades, nas que o suporte social é importante. Conclusão: conhecer e reflexionar sobre as percepções de pessoas com Doença de Parkinson sobre sua qualidade de vida contribui para a compreensão da doença e auxilia a proposta de intervenções clínicas adequadas para conseguir o cuidado integral. Sugere-se a revisão e adaptação do PDQ-39 ao contexto atual, os avanços tecnológicos e de conhecimentos sobre a Doença de Parkinson.
Palavras-chave: qualidade de vida, doença de Parkinson, PDQ-39.
Introduction
The complexity of Parkinson’s disease, and its secondary manifestations resulting from physical signs and symptoms, point to the need to discuss measures used to evaluate treatment success (1). Compromised mental, emotional, social, and economic circumstances affect the patient’s functioning and quality of life and that of the people around them, particularly caregivers (2, 3). Non-motor symptoms are considered incapacitating factors at all phases of the disease’s development. In addition, symptoms such as anxiety, depression, psychosis, sleep disorders, diminished impulse control, apathy, and cognitive dysfunction have been increasingly reported for patients with Parkinson’s disease (4, 5).
In recent years, traditional outcomes (efficacy, safety, survival, etc.) have been complemented by outcomes reported by patients themselves, including symptoms, adherence to treatment, adverse effects of medications, satisfaction with treatment and with healthcare services, functional status, and principally, quality of life (6, 7).
Quality of life is a subjective construct that includes those factors that substantially influence the life of a person, such as well-being, health, environment, income, and freedom, among others. According to the World Health Organization, quality of life is “an individual’s perception of life in the context of the cultural and value system in which they live, and in relation to their goals, expectations, standards, and concerns” (8).
The importance of evaluating quality of life results from valuing the perspective of the individual and from the capacity to estimate the functional and subjective impact of chronic diseases and their treatment on the lives of affected individuals from a multidimensional perspective (9).
Due to the progressive and chronic nature of Parkinson’s disease, one of the greatest challenges is to maintain the patient’s quality of life (10). In almost any area of their work, health professionals should evaluate patients’ perceptions of their own health because this perception is recognized as an indicator of their state of health. It measures patients’ perceptions of their physical and mental state, independent of medical interpretations of symptoms, and is a predictor of both mortality and the utilization of health services (11). For these reasons, self-perception has been increasingly valued in research, health planning, and decision-making by health teams (12). In addition, health professionals should identify strategies and adaptations that facilitate the management of symptoms by both patients and caregivers.
At the same time, quality of life in relation to health can be evaluated using generic instruments or instruments specific to each disease, and may include the patient’s physical, emotional, and social wellbeing and satisfaction with their state of health. Specific instruments are designed to study specific conditions or populations and have the advantage that they can detect particularities of quality of life in a particular situation on a specific and individual level (7, 9).
One of the tools frequently used to measure the quality of life of Parkinson’s patients is the Parkinson Disease Questionnaire-39, known as the PDQ-39. The PDQ-39 is made up of 39 questions categorized into in eight domains: mobility, daily living activities, emotional well-being, social support, stigma, cognition, communication, and bodily discomfort (13, 14). This instrument was developed and validated in 1995 and subsequently translated and validated in different languages, including Brazilian Portuguese (13, 15).
Progress in the treatment and accompaniment of Parkinson’s patients lead to reflections on the use of the PDQ-39 over time, and in different cultural contexts. Considering the central role that quality of life plays in caring for patients with neurodegenerative diseases, the intrinsic subjectivity and multidimensionality of the concept, and the methodological difficulties inherent to its evaluation, the objectives of this work are to identify matters related to quality of life from a patient perspective, compare them with the aspects considered in the PDQ-39, and describe the strategies adopted by patients to overcome their difficulties.
Materials and methods
Study design
A qualitative study developed using the focus group technique (16).
Selection and inclusion of patients
Participants in the study were selected intentionally by pharmaceutical professionals responsible to the Comprehensive medication management services, who had detailed knowledge about the characteristics of the patients being treated (17). The criteria for inclusion was that the patient should be responsible for his or her pharmacological treatment without the need for help from a caretaker. The presence of cognitive deficit as measured by the Mini-test of Mental State (Mini-exame do Estado Mental - MEEM) was a criterion for exclusion (18).
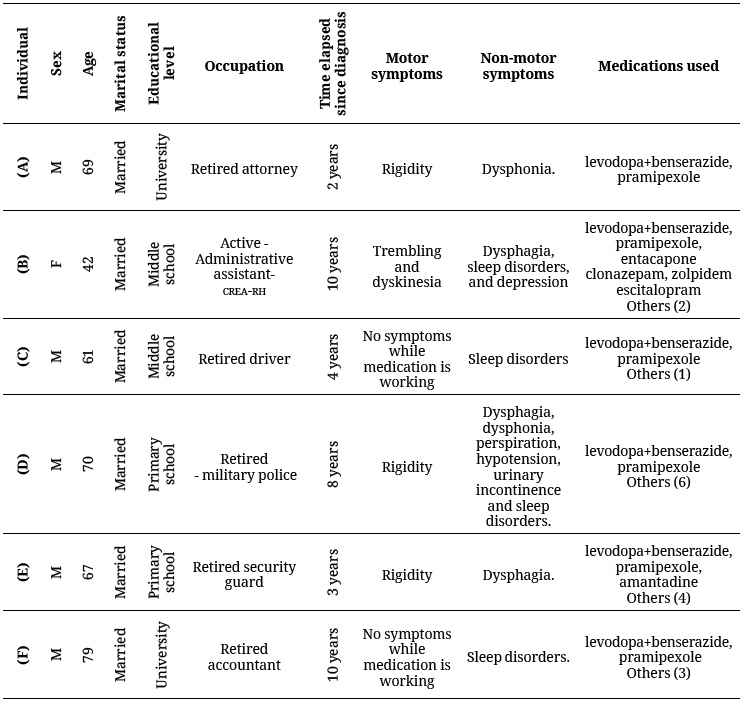
The focus group included patients with different characteristics. In order to form such a group, patients of both sexes, of different ages, and varying times elapsed since their diagnoses were invited to participate. Some of them had motor symptoms (tremor at rest, akinesia or bradykinesia, rigidity, postural instability, and gait disorders), and/or non-motor symptoms (neuropsychiatric manifestations, autonomic complications, and sleep disorders) (4, 19). Depression was identified when the patient mentioned that he or she had been diagnosed or when they had been prescribed medicines indicated for the treatment of depression. During the dispensing of medicine, patients were invited to participate in the focus group. The 6 patients who were invited agreed to participate; their characteristics are described in table 1.
Data collection
The study was carried out in April 2013, in the meeting room of a pharmacy associated with the public health system, where expensive medicines are distributed in Florianópolis, Brazil. The pharmacy also has ties to the Department of Pharmaceutical Science of the Universidade Federal de Santa Catarina, Brazil. The following people were present: the moderator, three observers (one of them acting as a recording secretary), and the six Parkinson’s disease patients. The moderator was a third pharmacist who also was knowledgeable about Parkinson’s disease, making it possible to identify areas of interest. The discussion of each individual topic was carried on until reaching a point of saturation, meaning that participants began to repeat themselves. Participants did not have friendship ties and did not know each other.
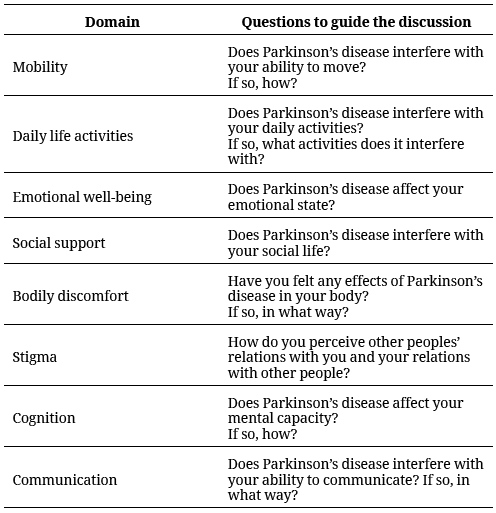
The discussion was guided with open questions that corresponded to the eight domains of the questionnaire for the evaluation of quality of life of Parkinson’s disease patients (PDQ-39) (15) (table 2). The focus group lasted about two hours. Participants were informed about the objectives of the project and told that an audio tape was being made of the discussion. All patients agreed to these conditions and signed the informed consent form before beginning their participation in the focus group.
Data analysis
The audiotape was transcribed and annotated with the help of notes taken at the session by the recording secretary and the other two observers. In order to maintain the anonymity of participants, they will be identified throughout this text by letters in alphabetical order. The material was analyzed using content analysis (20, 21). The data were codified, classified, and categorized by three independent researchers in order to avoid bias. The final categorization was reviewed by a fourth researcher in order to resolve cases where categorizations did not coincide. The domains included on the questionnaire PDQ-39 were adopted as a priori categories and the difficulties described by patients and strategies to overcome them in each case were adopted as subcategories. The difficulties mentioned by patients were compared with those considered on PDQ-39.
Ethical considerations
The study was approved by the Ethics Committee on Research with Human Subjects of the Universidade Federal de Santa Catarina in compliance with Act 1963 of 2011 and the standards established under Brazilian law (National Health Council Resolution 196 of 1996 (22). The study followed the international guidelines delineated in the Declaration of Helsinki and the Belmont report.
Results
In relation to Mobility, patients mentioned the following matters as responsible for diminished quality of life: slowness and difficulty of movement, difficulty placing purchases in bags, difficulty carrying shopping bags, tripping and falling, difficulty getting in and out of bed, and difficulty climbing stairs. In the domain of Daily living activities, patients said that their quality of life was compromised by difficulty writing, the frequency with which they broke dishes, difficulty brushing teeth, shaving, bathing, and combing their hair, difficulty cutting food, inability to drink liquid from a full container, inability to drive a car, and slowness in fastening their pants. The patients mentioned that both their mobility and their daily activities were more compromised at the beginning of the day, and that some symptoms were more intense on some days than on others. Some strategies used by patients to overcome these limitations included using an electric toothbrush, eating foods whose consumption did not require the use of fine motor skills, driving automatic cars, and receiving help from friends and family.
In the domain Emotional well-being, patients said that the following problems compromised their quality of life: insomnia, irritation, fragility, need for attention, and increased emotional sensitivity. Observers noted from the comments by patients that Parkinson’s disease affected their emotional state ―as evaluated on PDQ-39― but that their emotional state also affected their Parkinson’s disease. Some of the strategies mentioned by patients for alleviating their emotional suffering were talking about the disease, engaging in pleasurable activities, and talking to other people who also had the disease. One important point is that patients perceived that engaging in physical activity improved their mobility, their ability to carry out daily activities, and their emotional well-being.
In the domain of Stigma, the patients said that they were embarrassed to eat in public and angry that they had the disease. Some, however, mentioned the ease with which they could speak openly about the disease. In the domain of Social support, support and acceptance by families and participation in communities and support groups were mentioned as important tools for improving quality of life. It was observed, however, that some focus group participants resisted participating in support groups.
In the domain of Cognition, patients mentioned forgetfulness and reasoning difficulties as problems present in their day-to-day lives. It is important to note that these aspects were identified by patients who were diagnosed with Parkinson’s disease longer ago (between eight and ten years). In the domain of Communication, patients referred to slow and difficult speech, leading to poor diction, mangled words, breathy voices, and hoarseness. Some patients, however, did not bring up these limitations on communication caused by Parkinson’s disease as factors leading to a decreased quality of life, and no strategies were mentioned by patients for overcoming these difficulties.
In the domain of Bodily discomfort, patients mentioned cramps, cold extremities, body pain, and heavy feet as aspects of discomfort that affected them on a daily basis. Pain locations varied among the patients, and included waists, arms, and joints. Pain was most common in the evening and at night. One strategy used to alleviate this kind of pain was the use of hot compresses.
Most of the items present on PDQ-39 were recognized by the participants as factors related to quality of life. Not mentioned were difficulty tying shoes, being at home longer than desired, having to concentrate to watch television or read, or having disturbing dreams or nightmares.
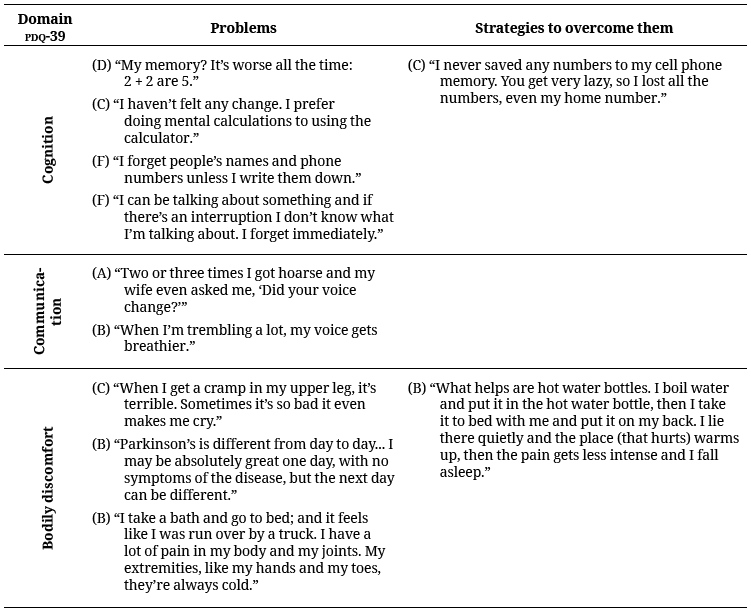
Table 3 presents excerpts that exemplify the problems identified by participants as compromising their quality of life, according to the categories mentioned on PDQ-39, as well as the strategies they used to overcome them.


Discussion
According to their responses, patients perceive many difficulties caused by Parkinson’s disease that affect the quality of life of sufferers, as is reflected in the literature (10, 23, 24, 25, 26). Within the domains mentioned on the PDQ-39, patients mentioned limitations on mobility and difficulty carrying out daily activities as a result of motor symptoms as the principal aspects that negatively influenced their perceptions of quality of life. This can be explained by the relation between the disease’s progression and progressively decreasing bodily mobility that results in increasing limitations on their ability to carry out daily activities (23, 24, 25, 26, 27). This affects the independence of Parkinson’s disease patients and often leads to the need for a caregiver (24, 25).
Participants also emphasized their emotional well-being. Emotional and social factors affect their disabilities, daily limitations, and perceived stigma (10). Patients perceived non-motor symptoms and their relation to motor symptoms, identifying them as responsible for the decreasing quality of life. This effect has been reported previously by Montel, Bonnet, and Bungener (26). Anxiety seems to be manifested at specific times in relation to Parkinson’s disease: immediately after the diagnosis, when problems of mobility appear, when the use of prescribed medicines produces on-off fluctuations of effectiveness, and when patients are no longer able to fulfill their accustomed social roles or demonstrate their accustomed social abilities (28).
Some symptoms described by patients are associated with depression, such as moodiness, irritability, anguish, and despondency. Many authors consider depression to be one of the primary factors responsible for Parkinson’s patients’ decreased quality of life. Depression negatively influences other physical and cognitive symptoms, indirectly contributing to social isolation (27, 29).
In relation to social support, it was found that family support is important in order to confront difficulties that arise in daily life. Some patients described living without family support, however, primarily because their families were unaware of the limitations that Parkinson’s disease imposed on them. Brazilian society considers the family to be a socially important unit for caring for the ill, and families have their own point of view on health and illness, their own attitudes, and their own way of providing care (30). Family dynamics change when a member falls ill and enters into a process of increasing dependency, and family roles change when one member in particular is designated as responsible for the care of the ill person (31). According to Falceto, Fernandes, and Wartchow, the family is always affected by the illness of one of its members and can organize itself to alleviate, maintain, or even aggravate the ill member’s symptoms (32).
It is important to note that only one female participated in this study, and in her responses, she mentioned consequences of the woman’s role in Brazilian culture. In our society, women assume the role of caregivers when another member of the family is ill (31, 33). When women need care, however, they cannot always count on getting the support they need, which is emotionally difficult for them (10).
In addition to family support, the support of friends and participation in mutual support groups are important tools in the process of facing Parkinson’s disease. According to Sluzki, there is strong evidence that stable, sensitive, active, and reliable social networks protect people from other illnesses, provide support and guidance, positively impact on the timely and appropriate utilization of health services, accelerate recovery, and improve survival rates (34). That is to say, they generate health. In the same way that the health of an individual can be affected by their social relations, the presence of a disease, especially a chronic or debilitating one, detracts from the quality of social interactions, and, in the long-term, reduces access to social networks (34).
In the focus group, participants mentioned the Santa Catarina Parkinson’s Association as well as patient communities in the social media (i.e. Facebook). The social support provided by these groups provides a tool for mutual assistance, the exchange of information, support at times of crisis, and participation in social events, all of which impedes the isolation of patients, thereby improving the state of their health (35, 36).
It was also observed that patient resistance to participating in support groups had more to do with the stigma of having Parkinson’s disease than with the participation in itself. The responses of participants verify that this stigma is associated with their own denial and rejection of the disease. The way that doctors present a diagnosis of Parkinson’s disease to patients can increase this stigma, since this event constitutes patients’ first contact with the disease. Support groups are even more important for these individuals and their participation should be incentivized by all healthcare professionals with whom they come into contact.
Only some of the patients who participated in the focus group perceived that their cognition suffered after their diagnosis with Parkinson’s disease, but all of them believed that cognitive symptoms affect the quality of life of Parkinson’s disease patients. According to Navarro-Petemella and Marcon, cognitive symptoms do affect the quality of life of individuals with Parkinson’s disease, and these symptoms become most prevalent as the disease progresses (10).
Bodily discomfort was frequently mentioned by the individuals with Parkinson’s disease. Body pain, cramps, and cold extremities were felt on a daily basis. Pain has been associated with Parkinson’s disease since it was first described. The discomfort is associated with motor symptoms, especially akinesia and rigidity (37).
The results of this study also demonstrate that patients play an active role in the process of health and illness and generate particular strategies to live with their disease and overcome the difficulties that arise as it progresses. For example, physical activity is mentioned by people with Parkinson’s disease as an element that improves their quality of life. This effect has been verified in other studies, which suggest that physical activity is a promising adjuvant treatment for alleviating motor symptoms as well as non-motor symptoms including mood disorders, cognitive effects, and sleep disorders (38, 39).
The results of the study also point to certain limitations of the PDQ-39 as a tool for evaluating quality of life. In the Emotional well-being domain, for example, one aspect mentioned by individuals in the focus group was that their emotional state was an important factor related to the manifestations of Parkinson’s disease symptoms, especially motor symptoms. On the PDQ-39, however, the domain of Emotional well-being refers exclusively to the effects of the disease on the lives of affected persons, not to how their emotional state affects the disease’s symptoms. Other questions regarding the validity of the PDQ-39 for measuring effects within this domain have been studied previously (40).
Also of interest was that some items on the PDQ-39 were not mentioned by participants as matters that determined quality of life. This may be because our knowledge about Parkinson’s disease has progressed subsequent to the creation and validation of the PDQ-39, particularly in relation to non-motor symptoms (13). There has also been technological progress, improved access to information, and better-designed products such as utensils and vehicles, among other things. Difficulty tying shoes, for example, was not mentioned by participants, perhaps because they use shoes without laces. The problem of being at home for longer periods than desired may be minimized by the availability of vehicle adaptations or improved urban transportation policies.
Thus, although the PDQ-39 is a specific instrument that has been validated, consolidated, and translated into Portuguese, it was found to lack some relevant categories in relation to the current panorama regarding Parkinson’s disease, demonstrating that it requires revision and updating as has been recommended by Jones et al. (40).
Taking this into account, studying and reflecting on the perceptions of Parkinson’s disease patients regarding their quality of life and the strategies they have developed to overcome the difficulties that they face as a result of the disease contribute to its understanding. This improved understanding will enable health professionals to provide more comprehensive patient care. We propose a revision of the PDQ-39 and its adaptation to today’s context, to the latest technological progress, and to our expanded knowledge of Parkinson’s disease.
Acknowledgements
The authors thank the Parkinson’s disease patients who participated in the study. Despite their personal difficulties, they made every effort to collaborate and bring it to fruition.
References
1. Gallagher DA , Lees AJ , Schrag A . What Are the Most Important Non-motor Symptoms in Patients with Parkinson’s Disease and are we Missing Them? Mov Disord. 2010; 25(15):2493-500. doi: 10.1002/mds.23394
2. Schenkman M, Zhu CW, Cutson TM, Whetten-Goldstein K. Longitudinal Evaluation of Economic and Physical Impact of Parkinson’s Disease. Parkinsonism Relat Disord. 2001;8(1):41-50.
3. Rodríguez-Violante MA, Cervantes-Arriaga A, González-Latapí P, Velázquez-Osuna S. Factores asociados a la calidad de vida de sujetos con enfermedad de Parkinson y a la carga en el cuidador. Neurología. 2015;30(5):257-63. doi: 10.1016/j.nrl.2014.01.008
4. Bernal-Pacheco O, Limotai N , Go CL , Fernandez HH. Non-motor Manifestations in Parkinson Disease. Neurologist . 2012;18(1):1-16. doi: 10.1097/NRL.0b013e31823d7abb
5. Kummer A, Teixeira AL. Neuropsychiatry of Parkinson’s Disease. Arq Neuropsiquiatr . 2009;67(3):930-9.
6. Den Oudsten BL , Van Heck GL , De Vries J . Quality of Life and Related Concepts in Parkinson’s Disease: A Systematic Review. Mov Disord. 2007;22(11):1528-37.
7. Farias CNF, Barbosa MED, Farias AQ. Avaliação da qualidade de vida relacionada à saúde em ensaios clínicos. En: Nita ME, Secoli SR, Nobre MRC, Ono-Nita SK, Campino ACC, Santi FM, Costa AMN, Carrilho FJ. Avaliação de Tecnologias em Saúde: evidência clínica, análise econômica e análise de decisão. Porto Alegre: Artmed; 2010. p. 42-9.
8. World Health Organization (WHS). The World Health Organization Quality of Life Assessment (WHOQOL): position paper from the World Health Organization. Soc Sci Med . 1995;41(10):1403-9.
9. Cruz LN. Medidas de Qualidade de Vida e Utilidade em uma amostra da população de Porto Alegre [tese de doutorado]. [Porto Alegre]: Universidade Federal do Rio Grande do Sul; 2010. URL: http://www.lume.ufrgs.br/handle/10183/69911
10. Navarro-Peternella FM, Marcon SS. Qualidade de vida de indivíduos com Parkinson e sua relação com tempo de evolução e gravidade da doença. Rev. Latino-Am. Enfermagem. 2012;2(20):1-8.
11. Santana P, Vaz A. Os serviços de saúde e as mulheres. In. Ministério da Saúde. Direção Geral da Saúde. A saúde da mulher. Lisboa: Direção Geral da Saúde (DGS); 1990. p. 131-65.
12. Ferreira P, Ferreira L. A medição de preferências em saúde na população portuguesa. Rev Port Saúde Pública. 2006;24(2):5-14.
13. Peto V, Jenkinson C, Fitzpatrick R, Greenhallr R. The development and validation of a short measure of functioning and well being for individuals with Parkinson’s disease. Qual Life Res . 1995;4(3):241-8.
14. Martinez–Martin P, Jeukens–Visser M, Lyons KE, Rodriguez–Blazquez C, Selai C, Siderowf A, et al. Health-Related Quality of Life Scales in Parkinson’s Disease: Critique and Recommendations. Mov Disord. 2011;26(13):2371-80. doi: 10.1002/mds.23834
15. Carod-Artal FJ, Martinez-Martin P, Vargas AP. Independent Validation of scopa-Psychosocial and Metric properties of the PDQ-39 Brazilian Version. Mov Disord. 2007;22(1):91-8.
16. Guix J. Analizando los “porqués”: los grupos focales. Rev Calidad Asistencial. 2003;18(7):598-602.
17. Foppa AA, Chemello C, Vargas-Peláez CM, Farias MR. Medication Therapy Management Service for Patients with Parkinson’s Disease: A Before-and-After Study. Neurol Ther . 2016; 7:1-15. doi: 10.1007/s40120-016-0046-4
18. Brasil. Ministério da Saúde. Cadernos de Atenção Básica. Normas e manuais Técnicos. Envelhecimento e Saúde da pessoa idosa. Brasília: Ministério da Saúde; 2006.
19. Samii A, Nutt JG, Ransom BR. Parkinson’s Disease. Lancet. 2004;363(9423):1783-93.
20. Laville C, Dionne J. A construção do saber. Belo Horizonte: UFMG; 1999.
21. Bardin L. Análise de conteúdo. Lisboa: Edições 70; 2006.
22. Brasil, Ministério da Saúde. Comissão Nacional de Ética em Pesquisa. Conselho Nacional de Saúde (BR). Normas regulamentadoras de pesquisa envolvendo seres humanos. Resolução n. 196/96 de 10 de outubro de 1996 - CNS. Brasília, DF, 1996.
23. Soh SE, McGinley JL, Watts JJ, Iansek R, Murphy AT, Menz HB, et al. Determinants of health-related quality of life in people with Parkinson’s disease: a path analysis. Qual Life Res . 2013;22(7):1543-53. doi: 10.1007/s11136-012-0289-1
24. Carod-Artal FJ, Vargas AP, Martinez-Martin P. Determinants of Quality of Life in Brazilian Patients with Parkinson’s Disease. Mov Disord. 2007;22(10):1408-15.
25. Silva FS, Pabis JVPC, Alencar AG, Silva KB, Navarro-Peternella FM. Evolução da doença de Parkinson e comprometimento da qualidade vida. Rev Neurocienc. 2010;18(4):463-8.
26. Montel S, Bonnet AM, Bungener C. Quality of Life in Relation to Mood, Coping Strategies, and Dyskinesia in Parkinson’s Disease. J Geriatr Psychiatry Neurol . 2009;22(2):95-102.
27. Silva JAMG, Dibai Filho AV, Faganello FR. Mensuração da qualidade de vida de indivíduos com a doença de Parkinson por meio do questionário PDQ-39. Fisioter Mov. 2011;1(24):141-6.
28. Rahman S, Griffin HJ, Quinn NP, Jahanshahi M. Quality of Life in Parkinson’s Disease: The Relative Importance of the Symptoms. Mov Disord. 2008;23(10):1428-34.
29. Camargos ACR, Cópio FCQ, Sousa TRR, Goulart F. O impacto da doença de Parkinson na qualidade de vida: uma revisão de literatura. Rev. Bras. Fisioter . 2004;8(3):267-72.
30. Cecagno S, Souza MD, Jardim VMR. Compreendendo o contexto familiar no processo saúde-doença. Health Sciences. 2004;26(1):107-12.
31. Caldas CP. Envelhecimento com dependência: responsabilidades e demandas da família. Cad. Saúde Pública. 2003;19(3):773-81.
32. Falceto OG, Fernandes CLC, Wartchow ES. O médico, o paciente e sua família. En: Duncan BB, Schimidt MI, Gilgliani ERJ. Medicina Ambulatorial: condutas em Atenção Primária baseada em evidências. Porto Alegre: Artmed; 2004. p. 115-24.
33. Karsch UM. Idosos dependentes: famílias e cuidadores. Cad. Saúde Pública. 2003;19(3):861-66.
34. Sluzki CE. A rede social na pratica sistêmica: alternativas terapêuticas. 2nd edition. São Paulo: Casa do Psicólogo; 2003. p. 37-85.
35. Minkler M. Building Supportive Ties and Sense of Community among the Inner-city Elderly: The Tenderloin Senior Outreach Project. Health Educ Q. 1985;12(3):303-14.
36. Andrade GRB, Vaitsman J. Apoio social e redes: conectando solidariedade e saúde. Ciênc. saúde coletiva. Ciência & Saúde Coletiva. 2002;7(4):925-34.
37. Letro GH, Quagliato EMAB, Viana AA. Pain in Parkinson’s Disease. Arq Neuropsiquiatr . 2009;67(3):591-4.
38. da Silva FC , Iop Rda R , Dos Santos PD , Bezerra LM , Gutierres PJ , da Silva R . Effects of Physical Exercise Based Rehabilitation Programs on Quality of Life in Parkinson’s Disease Patients: A Systematic Review of Randomized Controlled Trials. J Aging Phys Act. ;4(3):484-96. doi: 10.1123/japa.2015-0162
39. Reynolds GO, Otto MW , Ellis TD , Cronin-Golomb A . The Therapeutic Potential of Exercise to Improve Mood, Cognition, and Sleep in Parkinson’s Disease. Mov Disord. 2016;31(1):23-38. doi: 10.1002/mds.26484
40. Jones JD, Hass C, Mangal P, Lafo J, Okun MS, Bowers D. The Cognition and Emotional Well-being Indices of the Parkinson’s Disease Questionnair-39: What do they Really Measure? Parkinsonism Relat Disord. 2014;20(11):1236-41. doi: 10.1016/j.parkreldis.2014.09.014
Author notes
* Aline Aparecida Foppa, MScCorresponding author: alinefoppa@yahoo.com.br
** Claudia Marcela Vargas-Peláez, PhD
*** Fabíola Bagatini Buendgens, MSc
**** Clarice Chemello, PhD
***** Mariana Piva Fleury Charmillot, Farm
****** Marjorie Marin, Farm
******* Mayara Seemann, Farm
******** Mareni Rocha Farias, PhD
Conflict of interest declaration
This project was partially financed by two Brazilian organizations: the National Council for Scientific and Technological Development (Conselho Nacional de Desenvolvimento Científico e Tecnológico – CNPq) and the Coordinating Agency for Advanced Training in Graduate Education (Coordenação de Aperfeiçoamento de Pessoal de Nível Superior - Capes). The authors declare that they have no conflicts of interest.